
Advertisement

What parents need to know about the new Ontario sex-ed curriculum
The Ontario government has released the new sexual-education curriculum, which includes details of when and what students will be taught.
The province says the curriculum, for Grades 1 to 8, has been updated following feedback from the public and consultation with experts.
The Ministry of Education says the new 320-page Health and Physical Education Curriculum focuses on various topics including mental health, sexual health and consent.
It also examines the effects and risks of substance use, including cannabis and vaping.
The new curriculum replaces a much-criticized teaching plan brought in after the Progressive Conservatives took power last year.
The government has broken down what students will learn and when. Here’s a brief guide of what to expect and what’s changed:
- In Grade 1, students will be taught to identify body parts, including genitalia (penis, testicles, vagina and vulva)
- In Grade 1, students will be taught to use body-positive language
- In Grade 1, students will learn about habits and behaviour, including vaping
- In Grade 3, students will learn about the different types of legal and illegal substance use
- In Grade 5, students will learn to identify the factors that affect the development of a person’s self-concept, including their sexual orientation
- In Grade 5, students will learn about the negative effects of making homophobic comments
- In Grade 8, students will learn about gender identity (male, female, Two-Spirit, transgender) and learn more about sexual orientation (heterosexual, gay, lesbian, bisexual, pansexual, asexual)
- Under the former Liberal government’s plan, gender identity and sexual orientation was to be taught in Grade 6. It has been delayed until Grade 8
- In Grade 8, students will learn about abstinence, contraception and the use of suitable protection to prevent pregnancy and sexually transmitted blood borne infections (STBBIs)
- Parents can now opt their child out of sex-ed lessons with a new policy put into place – this must be completed by Nov. 30
- The new curriculum has a stronger and earlier emphasis on mental health, starting in Kindergarten
The new curriculum will go into effect at the start of the 2019 school year.
To view the full Health and Physical Education curriculum for Grades 1 to 8, click here.
Related Stories
- Ontario government releases new sex-ed curriculum
Toronto Top Stories

Several EB lanes of Hwy. 401 between Yonge and Bayview closed due to collision, fuel spill

Jacob Hoggard has begun serving prison sentence after appeal dismissed

Several Pusateri's Fine Foods grocery stores closing amid bankruptcy proceedings

Police charge woman who allegedly contaminated two Milton pools with feces, chocolate bars

Pedestrian hospitalized after hit-and-run in Scarborough

Jill Dunlop named Ontario's new education minister after Todd Smith resigns
Watch more from ctv news.

Building at risk to collapse causes evacuation

One dead, one injured in police-involved shooting

Jill Dunlop appointed as new education minister

Feedback Friday: Condo repair frustrations

Fatal police-involved shooting in Innisfil

Building in Kensington Market at risk to collapse
Consumer alert.

Toronto man denied rental car after trying to use prepaid credit card. Here is why not all businesses accept them.

These are the safest and most reliable used cars to buy

Shuttle ride in Mexico sets Ontario man back more than $3K. Here's what happened

'I have until next week': Toronto condo owner facing $40,000 bill for new windows

Best luggage for that late summer escape

U.S. loosens leash on rules for Canadian dogs crossing the border
Covid-19 in ontario.

'We are on the right track:' Toronto formally ends municipal state of emergency after 777 days

Local medical officers of health pen letter to Ontario's top doctor asking for mask mandates back

Ontario Liberals pledge to add COVID-19 vaccine to school immunization list
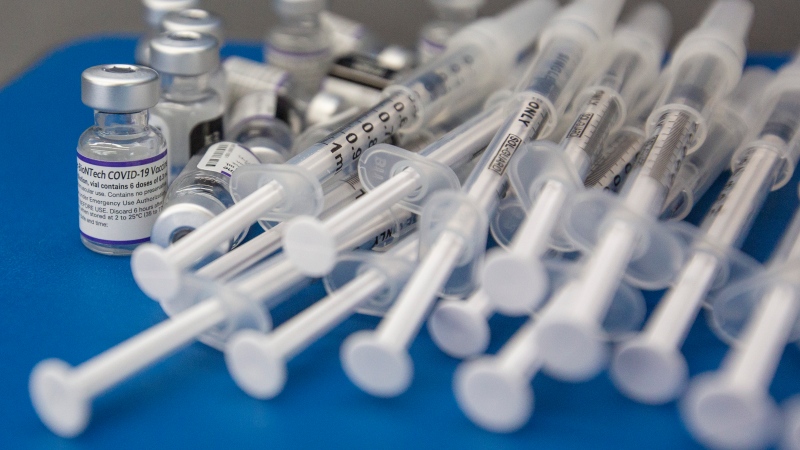
Nearly half of eligible Toronto residents have now received a fourth dose of COVID-19 vaccine

Will Toronto’s fun summer programs stick around as COVID restrictions ease?

Fourth doses in Ontario: When should you get one?
Ctvnews.ca top stories.

Manitoba RCMP investigating triple homicide in McCreary

Ukrainian forces left a path of destruction in Russia operation

Victoria mayor slams B.C. premier's comments on firefighter suspension

London, Ont.'s Tessa Virtue and husband Morgan Rielly welcome first child

Downtown Toronto building evacuated amid concerns that it could collapse: Toronto Fire

Boy pleads guilty to murder in stabbing death of 12-year-old girl in Toronto apartment

Six men rescued from boat fire by off-duty firefighter

Man runs 500km to participate in Windsor, Ont. beer mile

Warning: Moment boy alerts officer to mom in submerged car
Totally toronto.

What's new at the CNE this year? Here's what you need to know

Shake Shack officially opens first Canadian location in downtown Toronto

Toronto Blue Jays' Davis Schneider has always been an All-Star in the eyes of his sisters. Now, they want to make it official

500 units, 7 spots: Revisit visitor parking rules, Toronto councillors urge
You are currently offline. Please connect to the internet to view the latest information.
Canadian Guidelines for Sexual Health Education
The 2019 Canadian guidelines for sexual health education by Sex Information and Education Council of Canada (SIECCAN) are meant to be a guide for educators and policy makers when it comes to comprehensive sexuality education in Canada. The 2019 edition includes new content on the importance of comprehensive sex-ed in Canada, a list of key educators and settings important for access to comprehensive sex-ed, and benchmarks on providing STI prevention education and STI testing in schools.
- Share on Facebook
- Share on Twitter
This app features content from the Your Sexual Health Hub and is available if you are offline. To visit the full Action Canada for Sexual Health and Rights website, go to www.actioncanadashr.org.
Need to Talk to Someone?
For information about sexual and reproductive health, including pregnancy options, and for referrals to clinics and hospitals that provide reproductive health services, including abortion, anywhere in Canada, please call the confidential toll-free information and referral line between 9:00AM and 9:00PM EST Monday to Friday (Access Line closed weekends for the month of August.
Call the Access Line 1-888-642-2725
Prefer texting? 613-800-6757
General Inquiries
613-241-4474 [email protected]
Donor Inquiries 613-241-4474 x 10800 [email protected]
Media Inquiries 613-241-4474 x 13200 [email protected]
The Tyee is supported by readers like you
The tyee is supported by readers like you, grow independent media in canada, are you part of the tyee’s critical 1%.

Thanks for reading this article from The Tyee. I hope it added something to your day. If we haven't met yet, The Tyee is an independent, non-profit news outlet based in Vancouver, B.C. We've been around since 2003 and our team publishes original in-depth articles every single weekday.
You are able to access all of The Tyee's articles — free of charge — because our non-profit newsroom is supported by thousands of supporters of independent journalism. We call them Tyee Builders, and they contribute an amount that works for them.
Why do we call them "Tyee Builders"? Because they literally help build The Tyee. As our reader contributions grow, we invest all of it back into more original journalism, and adding more talented researchers, writers and editors to our team.
Only about 1 per cent of people who regularly read The Tyee contribute financially, but amazingly, that’s enough to cover half of our total budget. Just 1 per cent of people chipping in means that the other 99 per cent get to enjoy open access to fact-based journalism published by a trusted, independent news organization.
Public interest journalism is vital for our democracy, but the sad truth is that newsrooms across Canada are struggling, and laying off more and more journalists each year. Support from our readers means that we can keep our newsroom staffed, resourced, and showing up every day with new original stories that you won't read anywhere else. It also means that we are accountable to you first, not shareholders (we don't have any) or corporate backers (we don't have any of those, either).
Be a part of making Canadian media better and join Tyee Builders today. You choose the amount and frequency you give, and you can cancel at any time.
— Jeanette Ageson, publisher
You are using an outdated browser. Please upgrade your browser or activate Google Chrome Frame to improve your experience.
Gender + Sexuality
Sex education in bc’s schools: an explainer, what and when do kids learn about contraception, consent, abortion, gender identity and more a sex ed primer..

Akhila Menon is a journalism fellow with The Tyee through Journalists for Human Rights inaugural Enhanced Access for BIPOC Youth in Canadian Media program.
What do British Columbia’s youth learn about sex, sexual orientation and gender identity in school, when do they learn it and how is it taught? These are questions that affect the well-being of every child in the province — and fuel debate and political action among adults.
The questions are so charged that in the most recent school board elections across the province, 28 candidates ran under the banner of ParentsVoice BC, a group with strong Christian conservative ties opposed to the current sex education approach in public schools. Some socially conservative trustee candidates also opposed B.C.’s SOGI, or Sexual Orientation and Gender Identity directives, which help educators make schools inclusive and safe for students of all sexual orientations and gender identities.
Parents and students might understandably be confused and wanting more information. Which is why The Tyee interviewed several education experts and practitioners to create this explainer.
Why do we teach sex ed in schools?
Twenty per cent of all B.C. youth in Grades 7 to 12 are sexually active according to a 2018 Adolescent Health Survey .
Comprehensive sex education in the classroom has been shown to improve decision-making outcomes. “Comprehensive” is important here. UNESCO’s 2018 Technical Guidance on Sexual Education defines comprehensive sex ed as “learning about the cognitive, emotional, physical and social aspects of sexuality. It aims to equip children and young people with knowledge, skills, attitudes and values that will empower them to: realize their health, well-being and dignity; develop respectful social and sexual relationships; consider how their choices affect their own well-being and that of others; and, understand and ensure the protection of their rights throughout their lives.”
Students who’ve had comprehensive instruction are more likely to have their first experience of sexual intercourse later, to have sex less frequently, to have fewer sexual partners, to engage less in risky sex and to use contraception, according to UNESCO.
Several of the experts The Tyee spoke to for the story stated that sex education is a human right. Yet in 2013, the BC Adolescent Health Survey found that the majority of young British Columbians in its sample reported that they were not learning where to get tested for a sexually transmitted infection (57 per cent) or where to get emergency contraception if they needed it (52 per cent). Many had not learned where to get free condoms or contraception (38 per cent) or where to access birth control (47 per cent).
Such findings prompted the province to update its approach to teaching sex ed in schools.
The province’s Physical and Health Education, or PHE curriculum, was redesigned and implemented between 2016 and 2019, including new standards for sexual education, developed by a team of teachers from public and independent schools and government experts.
“The language in the current PHE curriculum [in terms of sexual health content] is meant to destigmatize mental and sexual health and ensure non-judgemental language is used,” a spokesperson for the Education Ministry told The Tyee. “Rather than talking about the risks of certain activities, the focus is on promoting overall healthy sexual decision-making.”
What are kids taught about sex and when?
Sex ed starts in elementary school and progresses in a “developmentally appropriate way” as students get older, the ministry told The Tyee.
Kindergartners are taught to respond to unsafe and/or uncomfortable situations and demonstrate respectful behaviour.
From first to third grade, some of the important elements of sex ed include establishing boundaries, such as saying no without guilt.
In Grade 5, students learn about “physical, emotional and social changes that occur during puberty, including those involving sexuality and sexual identity, and changes to relationships.”
The curriculum recommends that sixth, seventh and eighth graders are taught about practices that reduce the risk of contracting STIs, reliable sources of health information and awareness of how to respond to risky situations.
And in Grade 10, the learning standards include an emphasis on healthy sexual decision-making as well as the intricacies of healthy relationships.
Currently, topics on human sexuality and reproduction in the PHE curriculum are mandatory for all B.C. students from kindergarten to Grade 10.
However, precisely what they learn in sex ed classes depends on who is doing the instruction.
Who teaches sex ed in BC schools?
In secondary schools, it was supposed to be mainly gym teachers when the B.C. sex ed curriculum was moved from health and career to physical and health education in 2015. But often it's staff teachers or school counsellors who teach the curriculum and in many circumstances the responsibility is contracted out to independent sex ed facilitators.
In elementary schools, classroom teachers or resource teachers deliver the health-related curriculum, including the portions of it pertaining to puberty, the reproductive system, etc.
So what students are taught in sex ed can vary from one school to another?
Yes, significantly. “Individual school districts, schools and educators are responsible for determining resources used in classrooms and ensuring that they meet B.C.’s curriculum standards,” the Education Ministry spokesperson told The Tyee. So, each school district decides who does the sex ed teaching, including who might be contracted to do the job.
What might students be told about abortion, for example? Students in schools in Abbotsford, Langley and other nearby cities may be taught by facilitators from Advokate Life and Education Services. Advokate operates “crisis pregnancy centres” which actively counsel pregnant women against seeking an abortion.
Or consider how abstaining from sex is presented compared to explaining how to practice safe sex.
An Advokate job posting from August 2022 to hire a sex ed presenter requires the candidate to be “fully committed to Advokate’s vision, mission and values, including a commitment to teaching and affirming abstinence as the best way to avoid sexually transmitted infections and unplanned pregnancies.”
Research shows that an abstinence-only focus when teaching sex ed can contribute to shame and stigma.
Jared White, executive director of Advokate, told The Tyee that “part of healthy decision-making is recognizing that sex has adult consequences.” Teens engaging in premarital sex not only risk pregnancy and contracting disease, they go on to have higher rates of divorce, he claimed, citing a book his organization uses in teaching sex ed titled Hooked: The Brain Science of How Casual Sex Affects Human Development .
The Instagram account for Advokate’s sex-ed program Sexual Health and Integrity for Teens seeks to convince teens that if you have sex with someone who you decide you dislike, “Whether your [sic] like it or not you will naturally connect to that person.”
The Tyee shared the Advokate Sexual Health and Integrity for Teens presentation outline with Kristen Gilbert, a sex ed facilitator for over 18 years who is the education director for the non-profit Options for Sexual Health . Her judgement of the Advokate approach? “Rather than offering relevant, useful information on sexual decision-making, [they claim] that the opposite of abstinence is casual sex/sex addiction. They’re essentially offering abstinence-only education.”
Contrast Advokate’s offerings with how Saleema Noon, with the organization Sexual Health Educators, teaches sex ed in many Vancouver schools. Her “primary goal is to aid young people with the knowledge and the skills they need to enjoy their sexuality, both physically and emotionally, and stay safe and healthy. Whereas abstinence-only sex ed is fear-based. And problem-focused.”
“We start with the basics,” says Noon. “And we scaffold information as kids get older in a way that's relevant to their stage of development and their experience.”
For kindergarteners and first graders, the basics include a review of the three private parts of the body: mouth, breasts and genitals, as well as a discussion about consent. Students are taught the scientific terms related to anatomy and reproduction (i.e., vulva, penis, testicles, vagina, urethra, anus, uterus), that the baby is born through the vagina, and that families are formed in different, unique ways.
Tenth graders receive a more comprehensive three-hour session, split in two parts, that provides information about “healthy sexuality, self-care, safer sex, sexual decision-making, consent, healthy relationships and online safety.”
How Noon teaches evolves with the times, she adds. It’s important to adjust and ensure that the content being provided is relevant to young people’s lives, using language that is inclusive and helps every student feel seen and heard while being medically accurate, she says.
A comprehensive, inclusive sex ed program, according to Noon, makes no assumptions about, for example, penetrative vaginal sex being the only type of sex. It recognizes the breadth of sexual experiences, and how we're all unique, in terms of our sexual orientation and gender identity.
“We know from research that it delays sexual activity. Because it’s so much more than just having sex or not having sex,” she told The Tyee. “It’s about intimacy and communication and healthy relationships and connection, and pleasure and consent, and all that good stuff.”
Some B.C. school boards have attempted to standardize their sex ed courses. Vancouver’s trustees mandated that sex education delivery must be ethical and avoid a reflection of the facilitator's own values and present information that is unbiased and factual, for example.
Gilbert questions whether programs like Advokate’s would meet these standards.
Where is there room for improvement in BC’s sex ed curriculum?
As we’ve seen above, there can be a range of views on this one.
“Our curriculum is more current and reflective of the needs of students than many other provinces,” says sex ed facilitator Noon. “But it has become vaguer and less prescriptive in its learning objectives.” For teachers who are comfortable “running with it,” according to Noon, this is a good thing. “But there’s little guidance and support for teachers who may not be comfortable or don’t have as much experience teaching sex ed.”
“An ideal sex ed curriculum would be an evidence-based, comprehensive one,” says Brandy Wiebe, Noon’s colleague and a sexuality professor at the University of British Columbia.
Wiebe notes that while the current curriculum makes an effort to address issues around gender and sexual identities, “The tough thing about the curriculum is that it’s quite broad.”
Gilbert believes some of the content should be taught earlier. “According to the curriculum, I don’t talk about how babies are made until Grade 6,” she told The Tyee. “That is absolutely bananas. There are sometimes one or two kids in a Grade 6 or 7 class who I can tell by their faces are learning about it for the first time. And that’s far from ideal.”
She adds: “It isn’t harmful or inappropriate for children to understand how babies are made. It’s perfectly normal for children to be curious about this and it’s quite simple to explain using age-appropriate language.”
In addition, Gilbert says that being informed can help “protect children from abuse, as the parent can clarify the rules about touching, and establish themselves as an ‘askable adult’ who the child can come to with any concerns or questions.”
Predators who target children are more likely to look for a child who doesn’t know the rules about touching, and who hasn’t learned the scientific names for their body parts.
According to the 2018 Adolescent Health Survey , about 20 per cent of all girls surveyed, ages 12 to 19, had experienced sexual abuse.
Taylor Arnt, an MA student at UBC and participant in the Level Youth Policy Program comprising Indigenous and racialized immigrant and refugee youth across B.C., wrote a policy proposal for comprehensive sex ed in B.C. Arnt pointed out that the current curriculum doesn’t use the term “consent.”
The Tyee reported on this issue earlier this year.
“Schools need to explicitly mention the word consent in their sexual education lesson. It’s important that be included because, in cases of sexual violence involving the law, the issue of consent always comes up,” Arnt said.
Research backs up Arnt. A recent Canadian Women’s Foundation study found that 55 per cent of Canadians don’t fully understand consent when it comes to sexual activity.
A recent Ministry of Education press release mentioned updated health guides and the expansion of kindergarten-to-Grade-12 curriculum resources that will support educators in teaching consent with an age-appropriate and non-discriminatory approach in the classroom.
Starting in early 2023, “the province will offer additional learning sessions through Safer Schools Together for parents and students about consent, online safety and healthy relationships.”
What is the difference between sex ed and SOGI instruction in BC schools?
In the recent past, a number of socially conservative groups have voiced concerns about SOGI 1 2 3.
In an email interview with The Tyee, Reg Krake, the executive director for SOGI 1 2 3, clarified that while sex education and SOGI 1 2 3 are often confused, the latter is a set of tools and resources to help create safer and more inclusive schools for students of all sexual orientations and gender identities, rather than a set education program.
“[SOGI 1 2 3] includes policies and procedures, inclusive learning environments and age-appropriate teaching resources that are aligned to B.C.'s K-12 curriculum, and that are designed to be woven into the delivery of B.C.’s curriculum, not as additional requirements of the curriculum.”
When asked about the public response to SOGI 1 2 3, Krake said that as per their internal evaluation process, educators who are part of the SOGI Educator Network are increasingly reporting that they have both the support and resources needed to deliver SOGI-inclusive education in their school or district.
“Each year we have tens of thousands of people accessing tools and resources from our website to help them create safer and more SOGI-inclusive schools, which speaks to the need that SOGI 1 2 3 helps address within the education field,” he added.
SOGI 1 2 3 does not, as some have claimed, “take away” from delivering math, language, arts, social studies or other core elements of the curriculum.
A recent EGALE survey of 4,000 students found that 62 per cent of 2SLGBTQIA+ respondents reported feeling unsafe at school. Schools have a responsibility to create safe and inclusive spaces for all students and SOGI 1 2 3 helps achieve that, Krake said.
It encourages inclusivity — and all students need to see themselves reflected in the world around them and to be seen for who they truly are — so that they can be free to be their most authentic selves and live their best possible life.
Can parents prevent their children from learning about sex ed in school?
In instances where students and their parents feel that topics like reproduction and sexuality might cause discomfort if addressed in a classroom setting, there is the capacity for students with parental/guardian consent to learn about the topics by an alternative means, a spokesperson for the Ministry of Education told The Tyee.
However, “The alternate delivery policy does not allow students to opt-out of learning about these topics.”
Students are still expected, in consultation with their school, to demonstrate their knowledge of the topics arranged by alternative means.
White, who also ran for school trustee under the banner of Abbotsford ParentsFIRST in last month’s school board elections, strongly believes that parents should have an equal say in their children’s education.
“I think parents are typically the people who know their kids the best and love their children the most,” White said about his stance. “And they're in the best position to be able to guide their children when it comes to healthy sexual decision-making.”
He told The Tyee that many districts have policies that require parents to be informed when their children are receiving sex education in school. Informing parents of what their children are being taught will help them reinforce those things at home.
“I know a lot of parents don’t feel equipped to speak about it with their children. And it might be good for schools to go a step further and have evening or weekend sessions for parents, where the parents can be informed because they may also have some gaps in their own knowledge.”
Read more: Health , Education , Gender + Sexuality
Share article via email
Get the tyee's daily catch, our free daily newsletter., your privacy is important to us..
When subscribing to a newsletter edition you'll also get early notice on Tyee events, news, promotions, partner messages and special initiatives.
Further to the provision of the Personal Information Protection Act, personal information is kept confidential by TheTyee.ca and will not be sold, traded, released, shared or distributed to any other individuals, organizations or agencies without prior consent or notification.
Measures have been enacted to ensure the integrity of personal information and to protect it from misuse, loss or alteration. All information submitted to The Tyee is only available to employees or sub-contractors who are bound by agreement with The Tyee to keep the information private. E-mail addresses are only used for the purposes of Tyee-related correspondence or comment moderation.
If you have concerns related to your privacy please contact us at [email protected]
Tyee Commenting Guidelines
Comments that violate guidelines risk being deleted, and violations may result in a temporary or permanent user ban. Maintain the spirit of good conversation to stay in the discussion. *Please note The Tyee is not a forum for spreading misinformation about COVID-19, denying its existence or minimizing its risk to public health.
- Be thoughtful about how your words may affect the communities you are addressing. Language matters
- Challenge arguments, not commenters
- Flag trolls and guideline violations
- Treat all with respect and curiosity, learn from differences of opinion
- Verify facts, debunk rumours, point out logical fallacies
- Add context and background
- Note typos and reporting blind spots
- Stay on topic
- Use sexist, classist, racist, homophobic or transphobic language
- Ridicule, misgender, bully, threaten, name call, troll or wish harm on others
- Personally attack authors or contributors
- Spread misinformation or perpetuate conspiracies
- Libel, defame or publish falsehoods
- Attempt to guess other commenters’ real-life identities
- Post links without providing context
Most Popular
Edmonton police tracked a critic’s social media, most commented, former bc united donors are jumping to rustad’s conservatives, how to beat out the far right at the ballot, the allure of tim walz’s progressive populism, most emailed, reacting to ai: what would marshall mcluhan say, j.d. vance, the new prince of ‘poornography’, in kitsilano, the case of the beloved and broken pool.

Alberta’s New ‘Recovery Community’ Pushes Profit-based Treatment
Familiar faces from BC emerge as the UCP continues to shun harm reduction.

Internal documents show a special unit branded a defence lawyer ‘anti-police’ and closely monitored his online statements.

For Anti-heroes, Is This the End?
The days of the damaged yet relatable main character are in decline. ‘Deadpool & Wolverine’ shows why it’s time to lionize something new.

How Programs for Youth Could Stem the Tide of Toxic Drug Deaths
School-based interventions hold the potential to save lives, researchers say.

How Politicians and Corporations Are Wrecking Brat Summer
Charli XCX’s album of the summer has taken on a life of its own. How we got here.

Why Swimming While Black Is a Political Act
Decades of discrimination for racialized people makes the pool a fraught space. What does it take to turn the tide?

The Crisis Facing Alberta Wildlife
Expert biologists are being elbowed aside by politicians and special interests.
The real lesson from recent French and UK elections: progressives should work together.

Bringing Salmon Home to the Columbia River
An Indigenous-led, cross-border approach has seen great successes. But it needs BC and Canada’s ongoing financial support.

Reject the tech or try to tame it? We asked Jaqueline McLeod Rogers, an expert on the Canadian media philosopher.

An expert dives into the vice-presidential candidate’s false claims of an impoverished ‘hillbilly’ upbringing.
US Surgeon Sues Alberta Health Services, Alleging Dishonest, Bad Faith Treatment
The doctor claims a conflict of interest led to his botched hiring process and move from Alberta.
The Barometer
Has Meta’s News Ban Affected Your News Intake?
- Tell us more…
Take this week's poll

Parents can benefit as much as their kids from Ontario’s new sex ed
Associate Professor, Education, York University, Canada
Disclosure statement
Jen Gilbert receives funding from SSHRC.
York University provides funding as a member of The Conversation CA.
York University provides funding as a member of The Conversation CA-FR.
View all partners
In time for back-to-school 2019, the Ontario government released a revised health and physical education curriculum. Commentators have noted that despite Premier Doug Ford having stressed the need for an overhaul, the new curriculum is strikingly similar to the one from 2015 , prompting some to call it a backtrack of election promises.
But what is new is that the Ontario government is now touting an opt-out policy for parents who want to remove their children from certain lessons on human development and sexual health .
The new policy requires schools to implement a more detailed process to “ provide parents with a list of all Human Development and Sexual Health expectations by grade .” It also give parents at least 20 school days notice before students are taught human development and sexual health.
With regards to the new opt-out policy, there are significant concerns about potential threats to children’s access to inclusive, accurate sexual education. However, progressive responses that criticize the new parental opt-out policy must be careful to not get stuck inside the government’s framing of sex education as a potential violation of parents’ rights.
Parents as partners
The majority of parents in Ontario support progressive, inclusive and comprehensive sex education. A large study by Alex McKay, executive director of the Sex Information and Education Council of Canada, and colleagues found that 87 per cent of Ontario parents agreed that sexual health education should happen in schools . The study was conducted during earlier conflicts over the Ontario sex education curriculum.
Even the government’s own consultation process received overwhelmingly positive support for sex education in schools .
But what about the parents who don’t support the curriculum, and might be contemplating the opt-out?
Many advocates of progressive sex education oppose opt-out policies — and for good reasons.
Education researcher Lauren Bialystok, from the Ontario Institute for Studies in Education at the University of Toronto, for instance, writes that Ford’s olive branch opt-out policy to those at odds with liberal norms is about framing democratic policy-making as an adversarial struggle between “the people” and “the elite.”
Read more: Doug Ford's reboot of sex education in Ontario: Same as it ever was
She has argued that parents’ rights to determine how their children are raised shouldn’t override students’ right to learn about sexuality . I agree with her. However, my concern is that focusing now on the opt-out policy might reinforce the misleading belief that parents are only an obstacle to their children’s sex education.
Why, we might ask, are schools not concerned about parents who might complain or opt out if their children are not receiving a progressive — and inclusive —enough sex education? What would sex education look like if progressive sex ed advocates took those concerns more seriously?
Larger issues
Discussions of sex education should begin from the assumption that all parents are invested in their child’s education. Even when parents — conservative or liberal — have concerns about the sex education their child receives at school, they act out of love and care, not just political convictions.
The government has cynically positioned sex education as a potential violation of conservative parents’ rights. In response to this strategy, progressive advocates must be careful not to repeat and reinforce that antagonism.
I know of no studies documenting how many parents opt their children out of sex education in Canada. But qualitative research from the United States suggests the number is very small .
If sex ed advocates, researchers or educators acquiesce to the government’s framing of this issue and make the opt-out policy the problem, they may lose sight of the larger issues.
For instance: How can our society provide teachers with the resources to implement this curriculum? How will schools ensure all students, including racialized and Indigenous students, girls and LGBTQ students, are able to explore their ideas about sexuality and gender both in and out of the classroom?

Sex ed in the playground
Even still, sex education researchers and advocates know that sex education is never confined to a single class. Even as parents, politicians, educators and researchers debate what should or shouldn’t be included in a formal sex education curriculum, young people are taking the lessons they receive from their teachers out into the playground.
There, the formal curriculum is modified by the informal sex education students receive at school about gender and sexuality. Sex education happens in the cafeteria, locker room, on Instagram, in movies, through music and on Netflix.
Sex education includes all these teachers. And if schools are going to help young people navigate these lessons, both in and out of the classroom, they should enlist the help of parents.
Schools have a responsibility to offer students comprehensive, inclusive, medically accurate sexual health education regardless of who their parents are. But this mission is enhanced when schools, and sex education advocates, recognize parents as resources for sex education.
Let’s not be afraid of sending home notices about the sexual health education students will be receiving. Let’s invite parents to share their concerns and hopes with schools and teachers. Let’s opt parents into sex education. They may benefit from it as much as their kids.
[ Thanks for reading! We can send you The Conversation’s stories every day in an informative email. Sign up today. ]
- Sex education
- Parents and education
- Ontario education
- Back to school 2019
- sexual health curriculum

Casual Facilitator: GERRIC Student Programs - Arts, Design and Architecture

Senior Lecturer, Digital Advertising

Service Delivery Fleet Coordinator

Manager, Centre Policy and Translation

Newsletter and Deputy Social Media Producer
SOGI 1 2 3 project
Inclusion for Sexual and Gender Diversity
A professional competency for educators and teacher educators
by: Dr. Wendy Carr
date: September 18, 2019
If it is our responsibility as educators and teacher educators to teach inclusively, then shouldn’t inclusive practices for LGBTQ2+ students be a professional competency? This article outlines work undertaken in one faculty of education (UBC) to enhance its language, curriculum, and practices regarding sexual orientation and gender identity (SOGI).
If we believe it is our responsibility as educators and teacher educators to teach inclusively across all areas pertaining to human rights, including those related to sexual and gender diversity, then should this not be a professional competency? If so, how do faculties of education integrate this into their programs and cultures? This article outlines some of the work undertaken in one faculty of education to enhance its language, curriculum and practices regarding sexual orientation and gender identity (SOGI) and some of the lessons learned.
University of British Columbia’s (UBC) Faculty of Education has implemented an ambitious campaign since 2016 to raise awareness and build capacity and culture related to SOGI inclusion for its students, faculty and staff. This came about in part because of significant changes to federal and provincial human rights legislation, in part because recent studies (e.g. the 2015 Every Teacher Project 1 ) show that many teachers feel their university education did not prepare them for the SOGI diversity they encountered in schools, and in part because it was simply the right thing to do. The goal was and is to prepare knowledgeable, inclusive educators and improve the experience of those who may be marginalized because of their sexual orientation and/or gender identity in our programs, classrooms and workplaces.
None of this work has taken place in a vacuum. Our work augments earlier work within the Faculty of Education and complements the work of others, such as the UBC Institute of Gender, Race, Sexuality and Social Justice and the Office of Equity and Inclusion, to name a few.
The Faculty of Education embarked on an initial two-year project funded by Dr. Robert Quartermain 2 through the ARC Foundation. It was focused largely on the Teacher Education Program’s approximately 800 teacher candidates and also on growing awareness and understanding among faculty, graduate students and staff. Donor funding supplemented Dean Blye Frank’s support and allowed for the secondment of a school district-based SOGI-inclusion educator, Steve Mulligan, to coordinate the project and augment the work of faculty in teaching about and modeling inclusive practices.
Education and support for teacher candidates
All teacher candidates take an ensemble of required courses to prepare them as future educators. We worked with course instructors to integrate various aspects of sexual and gender diversity and inclusion into six of these courses, through lectures and/or seminars:
- “SOGI 101” in the Preparation for Practicum series
- SOGI inclusion in Human Development, Learning, & Diversity
- LGBTQ2+ student support in Supportive School & Classroom Environments
- Diversity and inclusion in Education, Schools and Social Institutions
- Trans literacies 3 in Literacy Practices and Assessment
- Gender identity support and teaching practices in Development & Exceptionality
We also offer presentations, panels and workshops for teacher candidates, faculty, graduate students, and others; they have addressed SOGI-inclusive curricula and resources, sexual health education for all students and all bodies, working with trans and non-binary students, and faith, family and SOGI-inclusion, among many other topics.
We host bi-weekly SOGI Alliance meetings for teacher candidates, similar to school-based Gender and Sexuality Alliances (GSAs). The group engages in various activities, such as event planning, resource sharing, practicum-related discussions and a professional book club as well as just coming together in a safe, welcoming space for LBGTQ2+ students and allies.
Engagement of faculty and faculty advisors
UBC faculty members and faculty advisors (adjunct faculty who supervise practicum placements) are invited to all seminars and some of the course-based presentations. As part of the faculty advisor orientation days in August, Steve Mulligan delivers a SOGI 101 workshop, similar to one for teacher candidates in September. The project coordinator also meets with faculty advisors prior to the long practicum to discuss issues related to teaching SOGI content and supporting LGBTQ2+ teacher candidates in their school placements.
A working group that includes faculty members, staff members, graduate students and the project director and coordinator meets regularly to plan and review events, resources and strategies. It oversaw the development of a number of resources for faculty, such as inclusion statements 4 for course outlines, planning for guest presenters and panelists, development of a podcast and online resource based on faculty interviews about inclusive practices, and an online collection of SOGI-inclusive resources.
Professional development of staff
We have held a series of staff workshops that focus on inclusive language and practices, policies and procedures for interacting with LGBTQ2+ students, staff and members of the public, and learning about the university processes and systems related to chosen names and pronouns, facilities and other areas where binaried, heteronormative practices may contribute to marginalization.
Engagement of local K-12 teachers and alumni
We linked with the UBC Alumni Engagement Office to offer two workshops for alumni in local community locations, which were very well attended: Rethinking Gender: How do we break free from stereotypes ? and The Power of Teaching for Diversity and Inclusion . We also offer two-day summer professional learning institutes for in-service educators and leaders. In 2017 and 2018, our topic was Safe is Not Enough: Sexual Orientation and Gender Identity education and leadership , attended by educators from across B.C. In July 2019, there were three institutes on each of the UBC Vancouver, UBC Okanagan and UBC West Kootenay campuses. 5
Outreach beyond the faculty
Since 2018 the project has expanded into a much broader initiative called SOGI UBC (again funded generously by Dr. Robert Quartermain) extending in outreach to other faculties and units on UBC campuses and in other universities, including work with Canadian faculties of medicine. In addition, we have created an online Inclusion for Gender and Sexuality Diversity: Professional competency module 6 that complements a recently developed free, massive open online course (MOOC) called Gender and Sexuality: Applications in society . 7 SOGI UBC parallels the provincial SOGI 1 2 3 network, 8 a Ministry of Education-supported initiative offering freely available online resources to support professional learning for educators and parents. Given that most of our graduating candidates will be teaching in B.C. schools, this connection is key to bridging what is learned at UBC and their future practice as educators.
Some lessons learned
The work to date has been enlightening in ways that show where we’ve grown and also where continued work is needed. Teacher candidates have been extremely open to learning how to be inclusive educators. Some of their feedback:
“This project has been a valuable asset to me during my experience as a teacher candidate. Through meetings, seminars, and events, my knowledge on a once-unknown topic is now much greater, and I feel much more prepared and knowledgeable moving forward as a new teacher.”
“Being part of the SOGI Alliance has provided me with a space to chat, voice concerns and get expert advice.”
“While I am no expert on the subject, I feel as though I have gained an interest and understanding in the topic.”
The curriculum mapping process taught us that, while there are many embedded instances of inclusive practice in our courses, these often depend on the instructor delivering the course or section. We also learned that course syllabi tell only a small part of what is taught and learned in courses. We still wonder: Is SOGI-inclusion supported across all courses? How are binaried or heteronormative perspectives taken up or challenged? Are LGBTQ2+ authors part of course reading lists? etc. Similarly, we wonder how sexual and gender minority candidates and their perspectives are and are not included, and how instructors and mentors confront or condone ongoing discrimination encountered in classrooms and/or on practicum.
We have endeavoured to use an intersectional lens in our work in order to ensure that the notion of identity is understood in multi-faceted ways. An upcoming project 9 supports teacher educators in building inclusive pedagogical practices to effectively and respectfully engage with Indigenous- and/or SOGI-inclusive perspectives, content and learning approaches. Using coaching, modeling, reflection and collaborative inquiry, we hope to enhance anti-oppressive teaching practices.
Mirroring the Faculty’s work in mental health literacy, 10 we know there is a literacy to be developed around SOGI inclusion that involves enhancing knowledge and understanding, reducing stigma and shifting language and attitudes. We also know that this work takes time and a desire to be part of these changes, so we continue to employ an invitational, educative approach to engage more and more of our community. There is definitely more work to do.
Provincial standards of teaching practice speak generally about student diversity, equitable treatment, and emotional and physical safety. The Association of Canadian Deans of Education Accord on Teacher Education 11 underscores social justice, equity and inclusion and the importance of challenging all forms of oppression and violence. As professional competencies are defined and refined, we believe that education faculties, teacher regulators and other education stakeholders need to integrate inclusive language and practices relative to gender and sexual diversity in order to ensure socially just environments for students and educators at all levels. Our hope is that the work at UBC can inspire and also be informed by what is happening on other campuses across Canada.
Photo: Courtesy Wendy Carr
First published in Education Canada , September 2019
1 C. Taylor, T. Peter, C. Campbell, et al. (2015). The Every Teacher Project: On LBGTQ-inclusive education in Canada’s K-12 schools – Final report , The Manitoba Teacher’s Society (Winnipeg, MB: 2015). https://egale.ca/wp-content/uploads/2016/01/Every-Teacher-Project-Final-Report-WEB.pdf
2 SOGI UBC is funded by the Jane Rule Initiative at UBC established by Dr. Robert Quartermain.
3 Trans Literacies workshops are offered by the UBC Institute of Gender, Race, Sexuality and Social Justice.
4 Course syllabus inclusion statements: http://teach-educ.sites.olt.ubc.ca/files/2018/07/Possible-Inclusion-Statements-for-Course-Outlines.pdf
5 UBC summer institutes: http://pdce.educ.ubc.ca/sogi-vancouver
6 Inclusion for Gender and Sexuality Diversity: Professional competency module . http://educ.ubc.ca/faculty-units/office-of-the-dean/initiatives/sogiubc
7 Gender and Sexuality MOOC by Dr. Janice Stewart: www.class-central.com/course/edx-gender-and-sexuality-applications-in-society-12333
8 SOGI 1 2 3: www.sogieducation.org
9 UBC Teaching and Learning Enhancement project led by Dr. Jan Hare & Dr. Wendy Carr.
10 Mental health literacy as conceptualized by Dr. Stan Kutcher and Dr. Yifeng Wei (Dalhousie): http://teenmentalhealth.org
11 ACDE Accord on Teacher Education: http://csse-scee.ca/acde/wp-content/uploads/sites/7/2018/05/Accord-on-Teacher-Education_Summary.pdf
Meet the Expert(s)
Dr. Wendy Carr
Professor of Teaching, Senior Advisor to the Dean, Faculty of Education, University of British Columbia
Dr. Wendy Carr, Professor of Teaching in Language and Literacy Education, is Senior Advisor to the Dean of the Faculty of Education, University of British Co...
1 /5 Free Articles Left
LOGIN Join The Network
It looks like you've read all of your free articles.
Join the EdCan Network
Join the EdCan Network now for unlimited access to thousands of online articles, to receive our print magazine and access special discount programs.
Thousands of courageous educators rely on our network for content and analysis that can support them working under the radar to reach every learner despite the limitations imposed by the system. You can too.
Not ready to join right now? Check out EdCan Wire for more free content.
It looks like this page isn't available in French.
IDEAS TO SUPPORT EDUCATORS : Subscribe to the EdCan e-Newsletter
Quality research, reports, and professional learning opportunities.
Language Preference Langue de correspondance English Français English Français
Language selection
- Français fr
Questions and Answers: Sexual Orientation in Schools
Table of contents.
- Preface and Acknowledgements
Introduction
- What do we know about sexual orientation?
- There are no sexual minority youth in my school. Why address these issues?
- Homophobia and Harassment
- Mental Health
- Other Health Risks
- What do I do if a student discloses their sexual orientation to me?
- What you can do
- In the Schools
- In the Community
- What can I do to support the parents/caregivers of sexual minority youth?
- How can I help to build the resiliency of sexual minority youth?
- Concluding Perspective
- Additional Resources
First published in 1994 and revised in 2003 and 2008, the Public Health Agency of Canada’s Canadian Guidelines for Sexual Health Education (Guidelines) were developed to assist professionals working in the area of health promotion and sexual health education in programming which supports positive sexual health outcomes. Feedback from a national evaluation of the Guidelines indicated the need for companion documents to provide more detailed information, evidence and resources on specific issues. In response, the Public Health Agency of Canada ( PHAC ) identified a ‘question and answer’ format as an appropriate way to provide information to educators and other professional working with school-aged populations. The Questions and Answers styled documents are intended to cover a range of topics reflecting current issues in sexual health education with school-aged populations, are evidence-based and use inclusive language as reflected in the Guidelines .
This document, Questions & Answers: Sexual Orientation in Schools , is intended to address the most commonly asked questions regarding the sexual orientation of youth in school settings. The goal of this resource is to assist educators, curriculum and program planners, school administrators, policy-makers and health professionals in the creation of supportive and healthy school environments for youth struggling with issues of sexual orientation.
Acknowledgements
The Public Health Agency of Canada would like to acknowledge and thank the many contributors and reviewers who participated in the creation of Questions & Answers: Sexual Orientation in Schools . The development of this document was made possible through the valuable input provided by experts working in the field of sexual health education and promotion across Canada, including the members of the Sexual Health Working Group of the Joint Consortium for School Health. A complete list of the external reviewers can be found online.
In addition, the Public Health Agency of Canada would like to acknowledge the staff of the Sexual Health and Sexually Transmitted Infections ( STI ) Section, Centre for Communicable Diseases and Infection Control, for their contribution to the development of this document.
In 1996, the Canadian Human Rights Act formally included “sexual orientation” among the prohibited grounds of discrimination and in 2009, Canada marked the 40th anniversary of the decriminalization of homosexual activity in Canadian law and legislation. Lesbian, gay, and bisexual individuals (collectively, sexual minorities) now have the same rights and responsibilities as all Canadian citizens. In the span of those forty short years, Canada has emerged as one of the most progressive Western countries in recognizing basic human rights of sexual minorities, including equal partner benefits, equal adoption and foster-parenting rights, non-discriminatory workplace policies, inclusive health care, and the legalization of same-sex marriage. Despite these measures of progress, individuals are still discriminated against on the basis of their actual or perceived sexual orientation Footnote 1 .
QUESTIONING: A person who is unsure of his or her sexual orientation.
These Questions and Answers are designed to support the implementation of the Canadian Guidelines for Sexual Health Education Footnote 2 . The Guidelines are based on evidence that broadly-based sexual health education should reflect the diverse needs and realities of all people in ways that are age-appropriate, evidence-based, scientifically accurate, rights-based, culturally sensitive, respectful and inclusive of sexual orientation and gender diversity. It is the view of the Guidelines that inclusive “sexual health education should be available to all Canadians as an important component of health promotion and services” Footnote 3 .
These answers to frequently asked questions about sexual orientation Footnote 4 in Canadian schools are based on evidence-based research. This resource is targeted at helping curriculum and program planners, educators (in and out of school settings), administrators, policy-makers, and health care professionals implement the current Guidelines to ensure that:
- sexual health educational programming is inclusive of the pressing health, safety, and educational needs of sexual minority and questioning youth;
the experiences of sexual minority youth are included in all facets of broadly-based sexual health education; and
educators, administrators, and school board personnel are provided with a more thorough understanding of the goals and objectives of broadly-based and inclusive sexual health education.
Page details
Ontario.ca needs JavaScript to function properly and provide you with a fast, stable experience.
To have a better experience, you need to:
- Go to your browser's settings
- Enable JavaScript
Human Development and Sexual Health education by grade
On this page skip this page navigation.
Below are details on what students will learn about human development and sexual health (Grades 1-8) and why these concepts are being taught at certain age levels.
When children know how to care for and use the correct names of their body parts, they build understanding and respect for themselves and their bodies and can communicate clearly and ask for help in case of illness, injury or abuse.
Students will learn:
- to identify body parts, including genitalia, by their proper names
- to use positive language when describing their bodies
- about their senses and how they function
- basic good hygiene habits (for example, washing your hands, using tissues)
Helping children to understand that their bodies will change (for example, losing baby teeth) can help them:
- prepare for and adjust to those changes
- appreciate what their bodies are able to do and perceive them positively
- communicate about these changes with a trusted adult if they ever feel confused
- the basic stages of human development (infancy, childhood, adolescence) and related body changes
- good hygiene habits for oral health (for example, brushing your teeth, flossing, visiting the dentist regularly)
- to appreciate what their bodies can do
To foster healthy relationships, students will learn what healthy relationships look like. Students also learn about what makes them unique and how to show respect for all.
- about characteristics of healthy relationships and consent (for example, accepting differences, listening, stating and respecting personal boundaries, being respectful, being honest, communicating openly)
- describe ways to respond to bullying and other challenges (for example, peer pressure, being left out)
- about factors and habits that can affect physical and emotional development (for example, safe environment, caring adults, feeling like you belong, appreciating what your body can do and building a healthy body image, sleep, food, physical activity)
- how visible differences (for example, skin, hair and eye colour, clothing, physical ability) and invisible differences (for example, learning abilities, cultural values and beliefs, different types of families) make each person unique
- ways of showing respect for differences in others
Today, children enter puberty earlier: on average, girls enter puberty between the ages of 8 and 13 and boys enter puberty between the ages of 9 and 14. Learning about puberty before students may fully experience it helps prepare young people for changes in their bodies, emotions and social relationships.
- the physical changes that happen during puberty, and the emotional and social impact these changes can have on a developing child
- how personal hygiene needs may change during puberty (for example, the increased importance of regular bathing)
By Grade 5, students have developed some self-awareness and coping skills, and have also learned critical thinking and reflective skills.
Puberty can be stressful and helping students to understand changes in their bodies can help them cope. Students will also continue to learn the importance of showing acceptance and respect for themselves and others, including those who may be entering puberty earlier or later than their peers.
- about factors that may affect the development of a person's understanding of themselves and their personal identity, including their sexual orientation (for example, body image, self-acceptance)
- about the reproductive system, and how the body changes during puberty
- about the process of menstruation and sperm production
- to describe emotional and interpersonal stresses related to puberty
As children grow older and enter adolescence, understanding how they and their peers may be affected by the many changes they are experiencing helps them build a healthy sense of who they are.
By Grade 6, students have developed more self-awareness and coping skills, as well as critical thinking and reflective skills, to solve problems and examine issues. They will apply these skills to learning about stereotypes and assumptions.
By examining and challenging these stereotypes and assumptions, they continue to learn about respect for others, and build self-confidence to build a foundation for healthy relationships.
- an understanding about the impacts of viewing sexually explicit media, including pornography
- the physical, social and emotional changes that may occur in adolescence (for example, body growth, skin changes, increasing influence of peers, increased intensity of feelings) and how students can build a healthy foundation for relationships
- to make decisions in their personal relationships that show respect for themselves and others, recognizing the importance of consent and clear communication
- how stereotypes — and assumptions about gender, race, sexual orientation, ethnicity, culture and abilities — can affect how a person feels about themselves, their feelings of belonging and relationships with others
- appropriate ways to respond to and challenge assumptions, stereotypes, homophobia and racism
Students need information and skills to make sound decisions about their health and well-being before they face a situation where they may need that information.
Research has shown that teaching about sexual health and human development does not increase sexual behaviour and can actually prevent risky activity.
- the importance of having a shared understanding with a partner about: reasons for delaying sexual activity until they are older, the concept of consent and how to communicate consent, and the need to clearly communicate and understand decisions about sexual activity in a healthy relationship
- to identify common sexually transmitted and blood borne infections ( STBBIs ) and describe their symptoms
- how to prevent STBBIs and avoid becoming a parent before they are ready, including delaying first intercourse and other sexual activities until they are older, and using condoms and other forms of protection consistently
- about the physical, emotional, social and psychological factors to consider when making sexual health decisions (for example, the risk of STBBIs or of becoming a parent before they are ready, emotional readiness, sexual orientation, moral and religious considerations, cultural teachings, and impact on other relationships)
- how relationships with others and sexual health may be affected by physical and emotional changes in puberty and adolescence
Students continue to build their understanding of factors that support positive, healthy choices, including building a deeper understanding and appreciation of themselves and their identity. Students are also exploring healthy ways to engage in evolving and new relationships.
Students will learn about:
- things that could affect someone's ability to make safe and healthy decisions about sexual activity
- sources of support with respect to sexual health (for example, parents, health professionals, in-school resources, local community groups and religious, spiritual, and cultural leaders)
- gender identity, gender expression and sexual orientation, and to identify factors that can help all young people to develop positive personal identities
- abstinence, contraception and consent in order to make safe and healthy decisions about sexual activity
- benefits, risks and drawbacks associated with relationships involving different degrees of sexual intimacy
< Back to my filtered results
Canadian guidelines for sexual health education
The Canadian Guidelines for Sexual Health Education provide guidance to educators and policy makers for the development and evaluation of comprehensive evidence-based sexual health education in Canada. The revised 2019 Guidelines include new content: a section documenting the importance of comprehensive sexual health education in Canada, Core Principles of Comprehensive Sexual Health Education, a list and description of appropriate educators and settings for the provision of comprehensive sexual health education, and benchmarks for the provision of STI prevention education and linking to STI testing in schools.
- Skip to main content
- Skip to "About this site"
Language selection
- Français
- Search and menus
Health Reports Where do 15- to -17-year-olds in Canada get their sexual health information?
by Michelle Rotermann and Alexander McKay

DOI : https://www.doi.org/10.25318/82-003-x202400100001-eng
What is already known on this subject?
What does this study add, introduction, definitions, strengths and limitations, correction notice.
In the article “ Mortality inequalities of Black adults in Canada ” published on June XX, 2022, an error was found in PPP.
The following correction has been made :
Sexual health education delivered in school, provided by parents, or provided by other formal sources has been associated most closely with increased rates of condom use and improvements in many other sexual risk behaviours. Friends and the internet are other information sources, although quality and accuracy are not always as high. Nationally representative Canadian data about where adolescents obtain their sexual health information are lacking.
Data and methods
Weighted data from the 2019 Canadian Health Survey on Children and Youth were used to examine the sources typically used to obtain sexual health information by 15- to 17-year-olds, as well as the prevalence and characteristics of adolescents reporting not having an adult to talk with about sexual health and puberty.
Most 15- to 17-year-olds in Canada reported having at least one source of sexual health information (96.6%). More than half identified school (55.6%) and parents or guardians (51.2%) as sources of sexual health information. The internet (45.9%), friends (36.2%), and health care professionals (20.9%) were other common sources. Whereas 61.2% of adolescents identified more than one source of sexual health information, 3.4% reported not having any source. Nearly 15% of adolescents reported not having an adult to talk with about sexual health or puberty. Differences in sources consulted and having an adult to talk with depended on many factors, including sexual attraction and/or gender diversity, sex, immigrant status, racialized status, lower-income status, strength of parent–adolescent relationship, region of residence, and mental health.
Interpretation
An improved understanding of the sources of sexual health information used by adolescents and identification of characteristics associated with adolescents reporting not having an adult to talk with could help develop strategies to improve sexual health outcomes via better access to sexual health promotion and educational resources.
sex-ed, sexuality education, contraception, condoms, puberty
Michelle Rotermann is with the Health Analysis Division, Analytical Studies and Modelling Branch, Statistics Canada, Ottawa. Alexander McKay is the Executive Director of the Sex Information and Education Council of Canada.
- Many studies assessing the efficacy of sexual health education indicate that it contributes to safer sex practices, including increased rates of condom or contraceptive use, fewer sexually transmitted infections, reduced teen pregnancies, delayed sex, and fewer sexual partners.
- The quality, accuracy and completeness of sexual health information can differ by source.
- Where adolescents get their sexual health information can influence their sexual behaviour.
- It provides updated information about sources of sexual health education for 15- to 17-year-olds in Canada.
- While 97% of adolescents reported having at least one source of sexual health information, some adolescents reported not having an informational source. Males, immigrants, residents of some regions, adolescents who are sexually and/or gender diverse, and some racialized populations could be more vulnerable to experiencing negative sexual health outcomes in the absence of more support and education.
Establishing healthy behaviours to prevent disease and support well-being is easier and more effective during childhood and adolescence than it is later in life. Adolescence is an important development period in which adolescents reach sexual maturity. It is also when youth, on average, begin engaging in sexual activities for the first time. Note 1 Because adolescents and young adults experience some of the highest rates of sexually transmitted infections (STIs) and unplanned pregnancies, Note 2 , Note 3 , Note 4 it is important to ensure access to appropriate resources and related sexual health information to support more knowledgeable decision making and the adoption of healthy sexual behaviours. Sexual health is a key component of overall health and well-being. Note 5
Sexual health education provided via formal instruction (sometimes called curriculum-based sexual health education programs) often includes information about the biological aspects of contraception, STI s, condom use, sexual identity, reproductive health, etc. Note 6 More recently, content on individual and interpersonal (e.g., self-acceptance, healthy relationships) aspects of sexuality has been incorporated. Note 5 Many studies assessing the efficacy of sex education or condom education programs, typically taught in school, find they contribute to safer sex practices, including increased condom or contraceptive use, fewer STI diagnoses, reduced teen pregnancies, delayed sex, fewer sexual partners, etc. Note 7 , Note 8 , Note 9 , Note 10 , Note 11 Parents and other family members are another common resource that can help adolescents with their sexual health questions, Note 12 , Note 13 , Note 14 although not all adolescents are comfortable talking with their parents. Note 15 Mothers tend to be more effective teachers than fathers; having discussed sex-related questions with them was associated with a small protective role by increasing rates of contraceptive and condom use.16 Other sources of sexual health information may not be as effective, Note 16 , Note 17 , Note 18 p and sometimes the quality, accessibility, and impact on outcomes differs. Note 15 For some sources, such as the internet, the quality and completeness of the information vary widely from comprehensive sexual health websites to pornography. In summary, where adolescents get their sexual health information is important and can influence their sexual behaviour. Note 12 , Note 17 , Note 18
The objective of this study was to update Canadian information about sources of sex education self-reported by adolescents and the related resource of having an adult to talk with about puberty and sexual health. This information can help to identify gaps and monitor changing access to sex information. Disaggregating results by sociodemographic and other characteristics can identify differences between groups.

Data sources
The cross-sectional 2019 Canadian Health Survey on Children and Youth (CHSCY) collected detailed data on the physical health, mental health and related determinants of children and youth in Canada. Note 19 The CHSCY used a sampling list frame created from the Canada Child Benefit (CCB) files. The CCB files contain a list of all program beneficiaries, along with their names and corresponding contact information. This list was used to directly select the random sample of children and youth. Data were collected using a primarily self-completed electronic questionnaire, although interviewer assistance via the telephone was also available. Collection took place from February to August 2019 and covered the population aged 1 to 17 years living in the 10 provinces and the 3 territories.
Excluded from the CHSCY ’s survey coverage were children and youth living on First Nations reserves and other Indigenous settlements in the provinces, in foster homes, or in institutions. The CHSCY covers approximately 98% of the Canadian population aged 1 to 17 years in the provinces and 96% in the territories.
Two questionnaires were administered. The first was administered to the person most knowledgeable (typically a parent) and the second was administered directly to the selected respondents aged 12 to 17 years. The overall CHSCY response rate was 52.1%, while that for the 6,915 respondents aged 15 to 17 years was 41.3%. The questions on the sources of sex information were asked only of the 15- to 17-year-olds. The study sample for having an adult to talk with about sexual health information excluded another 60 respondents because they did not answer the question. The sample used for the analyses on the different sources of sex education excluded 61 additional respondents because of non-response. For covariates, “not stated” responses were set to missing and excluded from the frequency analyses, with missingness varying from none (e.g., for the province or territory) to nearly 5% on the sexual and/or gender diversity measure.
Main outcomes
Not having an adult to talk with about sexual health, puberty, and sexual development was based on responses to the question: “If you had a question or concern about puberty, your sexual development or sexual health, is there an adult that you could talk with to get help or advice?”
Adolescents were also asked about the sources they used to obtain sexual health information: “Where do you typically get sexual health information?” Eight sources were provided, and respondents could select all that applied: (1) school, (2) a parent or caregiver, (3) friends, (4) printed books or pamphlets, (5) the internet, (6) a health care professional such as a doctor or nurse, (7) nowhere, and (8) other. Responses to these questions were used to distinguish adolescents who reported having at least one source of sexual health information from others who reported not having any source (i.e., nowhere). They were also used to examine the characteristics of adolescents reporting different sources of sexual health information.
The selection of covariates was guided by the literature and data availability in the CHSCY and included sociodemographic, adolescent, and adolescent-household characteristics.
Sex at birth was coded as male or female. Gender (referring to the current gender that may be different from sex assigned at birth) was coded in the CHSCY as male gender, female gender, and gender diverse and was based on answers provided by the adolescent. It is acknowledged that the gender response categories boy and girl (for children and youth) are preferable. Note 20 Preliminary analysis of the gender modality of CHSCY respondents found that over 99% of 15- to 17-year-olds in this study who were assigned male at birth also selected “male gender”. Similarly, nearly 99% of adolescents in this study who were assigned female at birth selected “female gender”. These results create some analysis challenges because of the small numbers of transgender and non-binary youth in the CHSCY . For that reason, a sexual and/or gender diversity variable was included to minimize data suppression and allow some analysis of the experiences of transgender and non-binary youth. This categorization follows the example set by another CHSCY study. Note 21 This composite variable combined each respondent’s self-reported sex at birth, gender and sexual attraction information. Sexual attraction was based on responses to the question: “People are different in their sexual attraction to other people. Which best describes your feelings? Would you say you are: 1: Only attracted to males, 2: Mostly attracted to males, 3: Equally attracted to females and males, 4: Mostly attracted to females, 5: Only attracted to females, 6: Not sure.” Adolescents who said they had at least some same-gender attraction and adolescents who were coded as transgender or non-binary were grouped together and compared with the subset of cisgender teens who reported they were only attracted to a different gender (Appendix Table A). Cisgender adolescents who were unsure about the target of their attraction (4% of all 15- to 17-year-olds) were coded as missing. Being unsure about their attraction did not result in the exclusion of any records pertaining to transgender adolescents, because group membership could be ascertained based on being transgender or non-binary, despite missing information about attraction. Other dimensions of sexual orientation (including sexual identity or behaviours) were not available in the CHSCY .
The CHSCY included the concept of racialized population using racial and cultural group information collected in accordance with the Employment Equity Act and its regulations and guidelines. Respondents who identified as non-Indigenous were asked to identify which ethnocultural population group they belonged to. Indigenous respondents were coded as missing for these variables. Thirteen response categories were available and used for two separate variables (racialized or non-racialized and non-Indigenous [White]) and five population groups (South Asian, Black, Chinese, non-racialized and non-Indigenous [White], and “other racialized” [composed of individuals identifying as Filipino, Arab, Latin American, Southeast Asian, West Asian, Korean, Japanese, groups not defined elsewhere, and people identifying multiple population groups]). Respondents were also categorized as immigrants or non-permanent residents versus Canadian-born people.
Indigenous identity was based on information provided by the adolescent. Respondents identifying as First Nations, Métis and Inuit were identified as Indigenous people. Further disaggregation was not possible because of limited sample size.
Canada does not have a coordinated sexual health curriculum. Note 22 Instead, each province or territory is responsible for its own programming. Geographic differences related to sociodemographics can also affect regional differences in the sources of sexual health information reported. Analyses were disaggregated by province or territory of residence where the sample allowed. In one analysis (Table 6), it was necessary to create a territories estimate (three territories combined), since the territory-specific estimates would have required suppression.
Household income (self-reported total from all sources and before taxes and deductions) was categorized as below the 2019 median market income of $58,300 (also called income before taxes and transfers in 2019 constant dollars) or at the median or above. Note 23
Family structure , describing the living arrangements of the adolescent, was categorized as living with two parents (biological, step, adoptive, etc.) or not living with two parents (other). The strength of the parent–adolescent relationship was based on information about how often the adolescent talked to their parents or guardians about what they did during the day. Adolescents could report having these exchanges regularly (most of the time or often) or irregularly (never, rarely, or sometimes).
The self-perceived mental health of adolescents was classified as fair or poor versus good, very good, or excellent based on responses to the question: “In general, how is your mental health?”
The number of hours of screen time was categorized as 0 to less than 3 hours, 3 to less than 7 hours, 7 to less than 14 hours, 14 to less than 21 hours, or 21 hours or more based on responses to the question: “In the past 7 days, how much time in total did you spend using any electronic device such as a mobile device, computer, tablet, video game console or television while you were sitting or lying down?”
Analytical techniques
Descriptive statistics using weighted data, adjusted for non-response, were used to examine the prevalence of nothaving an adult to talk with about sexual health, puberty, and sexual development and to study the sources adolescents typically used to obtain sexual health information by selected covariates. Bootstrap weights were applied to account for the underestimation of standard errors resulting from the complex survey design. Note 24 Analyses were performed using SAS 9.4 and SUDAAN 11.0.3. Differences between weighted estimates were calculated with t-tests. Reported differences in the text are statistically significant at the p < 0.05 level (meaning that they were not likely to have occurred by chance alone). To improve readability, the term “statistically significant” is not typically repeated.
Sources of sexual health information
According to the CHSCY , most 15- to 17-year-olds reported having at least one source of sexual health information (96.6%) (Tables 1 and 2). More than half of adolescents in Canada identified school (55.6%) and parents or guardians (51.2%) as sources of sexual health information (Table 2). The internet (45.9%), friends (36.2%) and health care professionals (20.9%) were also common sources. Books or other printed materials (7.0%) and other sources (1.7%) were less frequently cited.
More than 6 in 10 adolescents (61.2%) identified more than one source of sexual health information (Table 1). Just over one-quarter (25.8%) identified two sources, nearly one in five (18.7%) identified three sources, and one in six (16.7%) identified four or more sources. More than one-third (35.4%) of adolescents reported a single source, and 3.4% reported not having any (Table 1).
| Number of different sources | Total | Male | Female † | ||||||
|---|---|---|---|---|---|---|---|---|---|
| % | 95% confidence interval | % | 95% confidence interval | % | 95% confidence interval | ||||
| from | to | from | to | from | to | ||||
| 0 | 3.4 | 2.8 | 4.0 | 4.6 * | 3.7 | 5.7 | 2.1 C | 1.5 | 2.9 |
| 1 | 35.4 | 33.8 | 37.0 | 37.7 * | 35.5 | 40.0 | 33.0 | 30.8 | 35.2 |
| 2 | 25.8 | 24.4 | 27.4 | 25.9 | 23.9 | 28.0 | 25.8 | 23.8 | 27.9 |
| 3 | 18.7 | 17.5 | 20.0 | 17.0 * | 15.4 | 18.6 | 20.6 | 18.8 | 22.4 |
| 4 or more | 16.7 | 15.5 | 17.9 | 14.8 * | 13.3 | 16.5 | 18.6 | 16.9 | 20.4 |
| * * referrer †† referrer CC referrer 2019 Canadian Health Survey on Children and Youth. | |||||||||
While both males and females reported consulting many of the same sources for sexual health information, there were some differences by sex. For example, it was more common for males to report having one source (37.7% versus 33.0% for females) or no typical sources (4.6% versus 2.1% for females). Reporting three (20.6% for females versus 17.0% for males) or four or more (18.6% for females versus 14.8% for males) sources was more common among females.
Also, more males (58.5%) than females (52.7%) identified school as a source of sexual health information. However, higher percentages of females identified parents or guardians (55.7% versus 46.9% for males), friends (40.9% versus 31.7% for males), health care professionals (25.3% versus 16.7% for males), and books (7.8% versus 6.1% for males) (Table 2). The internet (45.2% for males versus 46.6% for females) and other sources (1.6% for males versus 1.7% for females) were identified by similar percentages of males and females.
| Sources identified | Total | Male | Female † | Sexually and/or gender diverse | Cisgender with exclusive different- gender attraction † | Immigrant or non-permanent resident | Canadian-born resident † | ||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| % | 95% confidence interval | % | 95% confidence interval | % | 95% confidence interval | % | 95% confidence interval | % | 95% confidence interval | % | 95% confidence interval | % | 95% confidence interval | ||||||||
| from | to | from | to | from | to | from | to | from | to | from | to | from | to | ||||||||
| School | 55.6 | 54.0 | 57.3 | 58.5 * | 56.2 | 60.8 | 52.7 | 50.3 | 55.0 | 53.7 | 49.8 | 57.6 | 56.2 | 54.3 | 58.1 | 61.9 * | 58.0 | 65.6 | 54.2 | 52.4 | 56.1 |
| Parent or caregiver | 51.2 | 49.6 | 52.8 | 46.9 * | 44.7 | 49.1 | 55.7 | 53.4 | 57.9 | 49.4 | 45.6 | 53.2 | 52.5 | 50.6 | 54.3 | 44.7 * | 41.1 | 48.5 | 52.6 | 50.8 | 54.4 |
| Internet | 45.9 | 44.3 | 47.5 | 45.2 | 43.0 | 47.4 | 46.6 | 44.3 | 49.0 | 58.3 * | 54.3 | 62.1 | 43.9 | 42.1 | 45.7 | 48.1 | 44.2 | 52.0 | 45.4 | 43.6 | 47.2 |
| Friends | 36.2 | 34.7 | 37.8 | 31.7 * | 29.7 | 33.9 | 40.9 | 38.6 | 43.1 | 39.7 | 35.9 | 43.6 | 36.2 | 34.5 | 38.0 | 34.9 | 31.3 | 38.6 | 36.4 | 34.7 | 38.1 |
| Health care professionals | 20.9 | 19.6 | 22.3 | 16.7 * | 15.0 | 18.5 | 25.3 | 23.4 | 27.4 | 25.9 * | 22.5 | 29.5 | 20.3 | 18.8 | 21.8 | 19.5 | 16.6 | 22.7 | 21.3 | 19.9 | 22.8 |
| Books or pamphlets (printed) | 7.0 | 6.3 | 7.7 | 6.1 * | 5.2 | 7.1 | 7.8 | 6.8 | 9.1 | 10.4 * | 8.3 | 12.8 | 6.3 | 5.5 | 7.1 | 7.8 | 6.2 | 9.8 | 6.6 | 5.9 | 7.5 |
| Other | 1.7 | 1.3 | 2.2 | 1.6 C | 1.2 | 2.3 | 1.7 C | 1.2 | 2.5 | 1.3 D | 0.8 | 2.3 | 1.8 | 1.4 | 2.4 | 1.7 D | 1.0 | 3.0 | 1.7 | 1.3 | 2.2 |
| Nowhere | 3.4 | 2.8 | 4.0 | 4.6 * | 3.7 | 5.7 | 2.1 C | 1.5 | 2.9 | 2.2 D | 1.2 | 3.8 | 3.0 | 2.4 | 3.7 | 3.7 C | 2.4 | 5.8 | 3.2 | 2.7 | 3.9 |
| * * referrer †† referrer CC referrer DD referrer 2019 Canadian Health Survey on Children and Youth. | |||||||||||||||||||||
Other characteristics of the adolescents were also associated with sources of sexual health information. For example, those who are sexually and/or gender diverse relied more on the internet (58.3%), health professionals (25.9%), and printed materials (10.4%) than their cisgender counterparts with exclusive different-gender attraction (43.9%, 20.3% and 6.3%, respectively) (Table 2). Among adolescents born outside Canada, over 6 in 10 (61.9%) reported getting sexual health information from school, and fewer than half (44.7%) relied on their parents or caregiver. The pattern was different with respect to these sources for Canadian-born adolescents, with fewer reporting school as a source (54.2%) and more reporting their parents (52.6%).
The amount of time adolescents spent online was also associated with identifying the Internet as a source of sexual health information (Table 3). For example, fewer than 3 in 10 adolescents who reported less than 3 hours of screen time per week (28.7%) identified the internet as a sexual health information source—about half the estimate (56.1%) for those reporting 21 or more hours of weekly screen time.
| % | 95% confidence interval | ||
|---|---|---|---|
| from | to | ||
| 45.9 | 44.3 | 47.5 | |
| Hours | |||
| 0 to less than 3 † | 28.7 | 23.9 | 34.0 |
| 3 to less than 7 | 38.5 * | 35.0 | 42.0 |
| 7 to less than 14 | 45.5 * | 42.2 | 48.7 |
| 14 to less than 21 | 48.4 * | 44.9 | 52.0 |
| 21 or more | 56.1 * | 52.9 | 59.3 |
| * * referrer †† referrer 2019 Canadian Health Survey on Children and Youth. | |||
There were also some geographic differences in identifying school as a source of sexual health information (Table 4). For example, 60.2% of adolescents living in Ontario and about two-thirds of adolescents from Manitoba (66.9%) and the Northwest Territories (66.7%) identified school as a typical source, significantly above the estimates for the rest of Canada (other provinces and territories combined). By contrast, 39.6% of adolescents from Quebec reported school as a source, which was significantly lower than the corresponding estimate for the rest of Canada.
| % | 95% confidence interval | ||
|---|---|---|---|
| from | to | ||
| Total | 55.6 | 54.0 | 57.3 |
| Province or territory | |||
| Newfoundland and Labrador | 57.9 | 50.5 | 64.9 |
| Prince Edward Island | 54.3 | 47.9 | 60.6 |
| Nova Scotia | 60.4 | 53.2 | 67.2 |
| New Brunswick | 53.5 | 46.4 | 60.4 |
| Quebec | 39.6 ‡ | 34.7 | 44.8 |
| Ontario | 60.2 ‡ | 58.2 | 62.1 |
| Manitoba | 66.9 ‡ | 59.6 | 73.4 |
| Saskatchewan | 60.5 | 53.4 | 67.2 |
| Alberta | 58.6 | 53.7 | 63.4 |
| British Columbia | 59.0 | 54.4 | 63.5 |
| Yukon | 63.7 | 51.8 | 74.1 |
| Northwest Territories | 66.7 ‡ | 55.5 | 76.2 |
| Nunavut | 65.5 | 48.7 | 79.2 |
| ‡ ‡ referrer 2019 Canadian Health Survey on Children and Youth. | |||
Prevalence of not having an adult available to talk with about sexual health or sexual development
According to the 2019 CHSCY , 14.9% of adolescents aged 15 to 17 in Canada reported not having an adult available to talk with about sexual health or puberty (Table 5). More males than females reported not having an adult available (16.6% versus 13.2%, respectively). A higher percentage of sexually and/or gender diverse adolescents compared with cisgender adolescents (with exclusive different-gender attraction) also reported not having an adult available (18.3% versus 13.2%, respectively).
| '000 | % | 95% confidence interval | ||
|---|---|---|---|---|
| from | to | |||
| 164.9 | 14.9 | 13.8 | 16.1 | |
| Sex at birth | ||||
| Male | 93.6 | 16.6 * | 15.1 | 18.3 |
| Female † | 71.3 | 13.2 | 11.7 | 14.8 |
| Sexually and/or gender diverse | 34.4 | 18.3 * | 15.6 | 21.4 |
| Cisgender with exclusive different-gender attraction † | 114.0 | 13.2 | 11.9 | 14.5 |
| Non-racialized and non-Indigenous (White) † | 83.8 | 11.2 | 10.0 | 12.5 |
| Racialized | 80.7 | 23.0 * | 20.7 | 25.5 |
| South Asian | 19.2 | 22.9 * | 18.7 | 27.7 |
| Chinese | 17.4 | 26.5 * | 21.2 | 32.6 |
| Black | 12.3 C | 21.4 C * | 15.2 | 29.2 |
| Other racialized | 31.8 | 22.2 * | 18.8 | 26.0 |
| Yes | 43.9 | 22.5 * | 19.4 | 26.0 |
| No (Canadian-born) † | 119.1 | 13.3 | 12.1 | 14.5 |
| Yes | 6.7 C | 13.4 C | 9.7 | 18.4 |
| No † | 157.6 | 15.0 | 13.9 | 16.2 |
| Less than $58,300 | 60.5 | 19.3 * | 17.1 | 21.8 |
| $58,300 or more † | 104.3 | 13.2 | 12.0 | 14.5 |
| Two parents † | 111.3 | 13.8 | 12.6 | 15.0 |
| Not two parents (other) | 50.6 | 17.8 * | 15.4 | 20.5 |
| Regularly † | 56.9 | 8.5 | 7.4 | 9.8 |
| Irregularly | 107.1 | 24.6 * | 22.5 | 26.8 |
| Fair or poor | 42.6 | 22.9 * | 19.9 | 26.1 |
| Good, very good, or excellent † | 122.2 | 13.4 | 12.2 | 14.6 |
| * * referrer †† referrer CC referrer 2019 Canadian Health Survey on Children and Youth. | ||||
Nearly one-quarter (23.0%) of racialized adolescents reported not having an adult to talk with about sexual health or puberty, more than double the estimate for their non-racialized and non-Indigenous (White) peers (11.2%). Similarly, a higher percentage of adolescents who were not born in Canada, compared with those who were, reported not having an adult to talk with (22.5% versus 13.3%, respectively). By contrast, the percentage of Indigenous respondents (13.4%) who reported not having an adult available to talk with about their sexual health or puberty was comparable to the estimate for their non-Indigenous peers (15.0%).
At 24.6%, the prevalence of not having an adult to talk with about their sexual health was about three times higher for adolescents who did not regularly talk about their day with their parents or guardians than it was among those who did (8.5%). Additionally, reporting not having an adult to talk with was more common among those from lower-income households (below the 2019 median market income of $58,300) (19.3%) and those not living with two parents (17.8%) than it was for adolescents from higher-income households (13.2%) and those living with two parents (13.8%).
Mental health was also related to reporting not having an adult available to talk with about sexual health or puberty. Adolescents who reported worse mental health were more likely to indicate not having someone to talk with than those who considered their mental health to be better (22.9% versus 13.4%, respectively).
There was some variation across the country, with about one in five adolescents in British Columbia reporting not having an adult available, significantly above the estimates for the rest of Canada (other provinces and territories combined) (Table 6). By contrast, fewer adolescents in New Brunswick (10.3%) and Nova Scotia(9.9%) reported not having an adult available, lower than the rest of Canada.
| % | 95% confidence interval | ||
|---|---|---|---|
| from | to | ||
| Canada | 14.9 | 13.8 | 16.1 |
| Newfoundland and Labrador | 12.3 C | 8.4 | 17.6 |
| Prince Edward Island | 13.4 C | 9.7 | 18.3 |
| Nova Scotia | 9.9 C ‡ | 6.4 | 14.9 |
| New Brunswick | 10.3 C ‡ | 6.8 | 15.3 |
| Quebec | 13.1 | 10.1 | 16.9 |
| Ontario | 15.4 | 14.0 | 16.8 |
| Manitoba | 14.3 C | 9.9 | 20.3 |
| Saskatchewan | 14.5 C | 10.3 | 20.1 |
| Alberta | 14.1 | 11.1 | 17.8 |
| British Columbia | 19.3 ‡ | 15.9 | 23.1 |
| Territories | 18.7 C | 12.6 | 27.0 |
| ‡ ‡ referrer CC referrer 2019 Canadian Health Survey on Children and Youth. | |||
Considerable research suggests that adolescents who have received sexual health education are better at making informed sexual health decisions, thereby contributing to healthier sexual development and safer sexual behaviours. Note 7 , Note 8 , Note 9 , Note 10 , Note 11 According to this study, most adolescents in Canada reported having access to sexual health information, and the majority had an adult to talk with about this topic.
People from racialized and some ethnic groups, and sexual minorities can be disproportionately affected by negative sexual and reproductive health outcomes. Note 4 , Note 25 , Note 26 , Note 27 , Note 28 Gaps in sexual health education for some populations may have contributed to these differences. The current study indicated, for example, that nearly twice as many foreign-born adolescents and adolescents from racialized population groups reported not having an adult available to discuss sex-related concerns as their Canadian-born or non-racialized and non-Indigenous (White) peers. Higher percentages of adolescents who are sexually and/or gender diverse versus their cisgender counterparts (with exclusive different-gender attraction) also reported not having an adult to talk with about sexual health. Youth who belong to some ethnic or racialized groups, who are immigrants, or who are sexually and/or gender diverse may not always have the understanding and support of family—therefore, they may not be able to discuss their sexual and reproductive health. Note 27 , Note 28 , Note 29 The provision of sexual health education at school, particularly if it is culturally sensitive and inclusive, can help ensure adolescents who might not otherwise have access to this valuable information can obtain it. Similarly, for adolescents born outside Canada, school can be an especially important source of sexual health information.
Results from this study align with others showing that any youth, regardless of sexual experience, sexual attraction, gender identity, race or ethnicity, can find talking with their parents about sex embarrassing. Note 17 , Note 30 Parents can also find these conversations challenging, owing to their limited knowledge, discomfort with the subject, or concerns about appropriateness or necessity. Note 31 This helps to explain why nearly half of adolescents do not identify their parents as a source. Talking regularly with parents does, however, seem to help foster communication between parents and children, Note 32 a finding echoed in this CHSCY study showing that adolescents who talked regularly with their parents were less likely to report not having an adult to talk with about their sexual health concerns.
Male and female adolescents also tended to differ in where they obtained their sexual health information. Females tended to rely more often on their parents, friends and health professionals, whereas more males reported school as a source. Also, not having an adult to discuss their sexuality questions with was more than twice as common among males than females. Other research suggests that this sex difference can matter because the subjects covered have been shown to differ depending on the provider and sex of the recipient (e.g., more females receive guidance on how to say no and where to obtain birth control, whereas males are more likely to learn how to use condoms). Note 13 , Note 33 , Note 34 These sex differences can put adolescents not receiving a more complete sexual health education curriculum at risk.
This study found some regional differences in the reporting of school as a source of sexual health information and in the rates of not having an adult to talk with about this topic. Education is a provincial or territorial responsibility; as a result, the curriculum is not standardized and varies across Canada. For students aged 17 in Quebec, the existence of pre-university and vocational career programming offered by Collège d'enseignement général et professionnel (CEGEP) might mean courses with sexual health education content are not always taken. This could help explain the lower numbers of Quebec adolescents reporting school as a source, although other factors may also have contributed.
This short study has several strengths, including that the CHSCY is a national, population-based survey that covers a wide range of subjects, allowing for a detailed look into the health and sociodemographic characteristics of Canadian adolescents’ use of different sources of sexual health information. Nevertheless, results of this study should be interpreted in light of several limitations.
Some variables relevant to the study of sexual health and related information were not collected by the CHSCY , including religiosity, Note 33 details about the sexual health education provided, the timing of the sexual health education, and information about an adolescent’s previous sexual behaviours and experiences.
The data are cross-sectional and thereby permit the observation of associations between variables at only one point in time. Information was self-reported and has not been verified, and it can be subject to recall and social desirability biases. The use of survey weights adjusted for non-response helped to ensure that the dataset more accurately represented the target population.
While the CHSCY was designed to study the health of children and youth and boasts a comparatively large sample, the problem of small sample sizes was not completely eliminated. This issue sometimes necessitated the use of dichotomized variables and meant the study could not examine certain at-risk and understudied subpopulations, including people with intellectual disabilities, Note 35 people with autism, Note 36 and Two-Spirit, Lesbian, Gay, Bisexual, Transgender, Queer and/or Questioning + (2SLGBTQ+) adolescents. Note 27 Disaggregated data about gender and sexual diversity can be of lower quality if the collected sample size is too small. In such cases, it is helpful to combine gender and sexually diverse respondents to produce estimates related to the broader 2SLGBTQ +population. Small samples or effect sizes in other parts of the analysis may also have affected significance testing.
Concluding remarks
This study provides an updated picture of the sources used by adolescents in Canada to obtain sexual health information. It also examines the characteristics of adolescents who reported not having an adult to talk with about their sexual health or puberty. While the majority reported having access, there were some adolescents who reported not having an adult they could talk with or another informational source. Adolescents who were male, were born outside Canada, were sexually and/or gender diverse, were racialized, were experiencing fair or poor mental health, were from lower-income households, talked infrequently with their parents, and resided in some regions could be more vulnerable to experiencing negative sexual health outcomes in the absence of more support and education. The differences identified in this study could help develop more tailored curricula or other resources to help all adolescents have the information and support they need to make more informed choices about sex.
| Value assigned to sexually and/or gender diverse variable | |||
|---|---|---|---|
| Yes | No | Missing | |
| Among adolescents who reported their gender as male and | |||
| their sex at birth as male (cisgender), and their sexual attraction as: | |||
| Only, somewhat, mostly, or equally attracted to males | ✓ | Note ...: not applicable | Note ...: not applicable |
| Only attracted to females | Note ...: not applicable | ✓ | Note ...: not applicable |
| Not sure | Note ...: not applicable | Note ...: not applicable | ✓ |
| Only, somewhat, mostly, or equally attracted to females | ✓ | Note ...: not applicable | Note ...: not applicable |
| Only attracted to males | ✓ | Note ...: not applicable | Note ...: not applicable |
| Not sure | ✓ | Note ...: not applicable | Note ...: not applicable |
| Among adolescents who reported their gender as female and | |||
| their sex at birth as female (cisgender), and their sexual attraction as: | |||
| Only, somewhat, mostly, or equally attracted to females | ✓ | Note ...: not applicable | Note ...: not applicable |
| Only attracted to males | Note ...: not applicable | ✓ | Note ...: not applicable |
| Not sure | Note ...: not applicable | Note ...: not applicable | ✓ |
| their sex at birth as male (transgender), and their sexual attraction as: | |||
| Only, somewhat, mostly, or equally attracted to males | ✓ | Note ...: not applicable | Note ...: not applicable |
| Only attracted to females | ✓ | Note ...: not applicable | Note ...: not applicable |
| Not sure | ✓ | Note ...: not applicable | Note ...: not applicable |
| Among adolescents who reported their gender as gender diverse and | |||
| their sex at birth as male and their sexual attraction as: | |||
| O nly, somewhat, mostly, or equally attracted to females | ✓ | Note ...: not applicable | Note ...: not applicable |
| Only, somewhat, mostly, or equally attracted to males | ✓ | Note ...: not applicable | Note ...: not applicable |
| Only attracted to males | ✓ | Note ...: not applicable | Note ...: not applicable |
| Only attracted to females | ✓ | Note ...: not applicable | Note ...: not applicable |
| Not sure | ✓ | Note ...: not applicable | Note ...: not applicable |
| their sex at birth as female and their sexual attraction as: | |||
| Only, somewhat, mostly, or equally attracted to females | ✓ | Note ...: not applicable | Note ...: not applicable |
| Only, somewhat, mostly, or equally attracted to males | ✓ | Note ...: not applicable | Note ...: not applicable |
| Only attracted to males | ✓ | Note ...: not applicable | Note ...: not applicable |
| Only attracted to females | ✓ | Note ...: not applicable | Note ...: not applicable |
| Not sure | ✓ | Note ...: not applicable | Note ...: not applicable |
| ... not applicable 2019 Canadian Health Survey on Children and Youth. | |||
More information
Note of appreciation.
Canada owes the success of its statistical system to a long-standing partnership between Statistics Canada, the citizens of Canada, its businesses, governments and other institutions. Accurate and timely statistical information could not be produced without their continued co-operation and goodwill.
Standards of service to the public
Statistics Canada is committed to serving its clients in a prompt, reliable and courteous manner. To this end, the Agency has developed standards of service which its employees observe in serving its clients.
Published by authority of the Minister responsible for Statistics Canada.
© His Majesty the King in Right of Canada, as represented by the Minister of Industry, 2024
Use of this publication is governed by the Statistics Canada Open Licence Agreement .
Catalogue no. 82-003-X
Frequency: Monthly

Sex Information & Education Council of Canada

New Release: The HPV Vaccine: Men, it's about time! Protect yourself AND your partner(s) from HPV-related cancers and genital warts.

Exciting News: Launch of New Gender-Based Violence Prevention Sexual Health Education Tools!

Just released: I'm a millennial woman: Should I get vaccinated for HPV?

SEXUAL HEALTH PROMOTION WITH DISABLED YOUTH TOOLKIT: LAUNCHED!
Latest SIECCAN News

SIECCAN updates
Delivered to your inbox, sign up to be notified of new announcements, surveys, resources and more, our partnerships and collaborations.
We are committed to building on existing partnerships and establishing new partnerships and collaborations based on shared objectives.

Visit our Promising Practices Portal to access comprehensive, up-to-date Canadian sexual health resources and educational materials.
Consultez notre portail des pratiques prometteuses, pour des ressources et du matériel actualisés d’éducation à la santé sexuelle..

Check out some of our latest projects...

The Sex Information & Education Council of Canada (SIECCAN) is a not-for-profit charitable organization established in 1964 that works with health professionals, educators, community organizations, governments, and corporate partners to promote sexual and reproductive health.

An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- Paediatr Child Health
- v.18(2); 2013 Feb

Language: English | French
Sexual knowledge of Canadian adolescents after completion of high school sexual education requirements
Maya m kumar.
1 Department of Pediatrics, Schulich School of Medicine and Dentistry; London, Ontario
Rodrick Lim
2 Pediatric Emergency Medicine, London Health Sciences Centre; London, Ontario
3 Children’s Health Research Institute, University of Western Ontario; London, Ontario
Cindy Langford
Jamie a seabrook, kathy n speechley.
4 Department of Epidemiology and Biostatistics, Schulich School of Medicine and Dentistry, London, Ontario
Timothy Lynch
Background:.
Formal sexual education is a mandatory component of the high school curriculum in most Canadian provinces. The present study was a preliminary assessment of sexual knowledge among a sample of Ontario adolescents who had completed their high school sexual education requirements.
A questionnaire, testing understanding of the learning objectives of Ontario’s minimally required high school sexual education course, was distributed in a paediatric emergency department to 200 adolescent patients who had completed the course.
Respondents demonstrated good understanding of pregnancy physiology and sexually transmitted infections, but poor understanding of concepts related to reproductive physiology, contraception, HIV/AIDS and sexual assault. Most respondents could not identify Canada’s age of sexual consent.
CONCLUSIONS:
Respondents demonstrated concerning gaps in sexual knowledge despite completion of their sexual education requirements. Further studies must determine whether a representative, population-based student sample would exhibit similar findings. Sexual education currently offered in Ontario may require investigation.
HISTORIQUE :
L’éducation sexuelle est un élément obligatoire du programme d’études secondaires de la plupart des provinces canadiennes. La présente étude visait à obtenir une évaluation préliminaire des connaissances en matière de sexualité d’un échantillon d’adolescents ontariens qui avaient terminé leur cours d’éducation sexuelle au secondaire.
MÉTHODOLOGIE :
Lors de leur visite au département d’urgence pédiatrique, 200 patients adolescents qui avaient terminé leur cours d’éducation sexuelle ont reçu un questionnaire afin de vérifier leur compréhension des objectifs d’apprentissage du cours d’éducation sexuelle de base offert dans les écoles secondaires de l’Ontario.
RÉSULTATS :
Les répondants ont démontré une bonne compréhension de la physiologie de la grossesse et des infections transmises sexuellement, mais une mauvaise compréhension des concepts liés à la physiologie de la reproduction, à la contraception, au VIH-sida et aux agressions sexuelles. La plupart des répondants ne pouvaient pas préciser l’âge du consentement sexuel au Canada.
CONCLUSIONS :
Les répondants ont démontré des lacunes préoccupantes en matière de connaissances sexuelles, même s’ils avaient terminé leur cours d’éducation sexuelle obligatoire. D’autres études devront déterminer si un échantillon d’étudiants représentatifs en population donnerait des résultats similaires. Les cours d’éducation sexuelle actuellement offerts en Ontario méritent peut-être d’être évalués.
Adolescence is a crucial period for learning about healthy sexuality ( 1 , 2 ). As teenagers struggle to complete the developmental tasks of adolescence, such as accepting their changing bodies and defining their sexual identities, they are at risk for negative sexual consequences ( 3 ). Sexually active Canadian teenagers commonly engage in risky sexual behaviours, including unprotected sex, multiple sexual partners and intercourse, before 15 years of age ( 4 ). Canadians 15 to 24 years of age also have the country’s highest incidences of chlamydia and gonorrhea infections ( 5 ). Such statistics raise concerns about whether young Canadians have sufficient knowledge to make responsible sexual decisions. Comprehensive sexual education for adolescents effectively reduces the incidence of negative sexual outcomes ( 6 , 7 ). The Canadian Paediatric Society and the American Academy of Pediatrics ( 8 , 9 ) recommend that paediatricians participate in the development and implementation of comprehensive sexual education programs in schools.
In Canada, education is under provincial jurisdiction and almost every province’s high school curriculum contains formal sexual education. Within the province of Ontario, sexual education is a subcomponent of health and physical education courses; each course is comprised of approximately 110 h of instruction. However, only a fraction of course time, determined by each school, is dedicated to sexual education; consequently, there is potential for significant variability among schools. Ontario’s Ministry of Education has outlined six course expectations ( Table 1 ) for its Grade 9/10 Healthy Growth and Sexuality unit ( 10 ). Completion of this unit is the minimum sexual education required for a high school diploma or certificate in Ontario.
Course expectations for Ontario’s Grade 9/10 Healthy Growth and Sexuality course ( 10 )
There are currently no standardized examinations or evaluation processes to assess the knowledge of students who have completed their sexual education requirements and no other standardized assessments of sexual education quality.
Several studies have attempted to assess the sexual knowledge of Canadian adolescents. The majority of these studies, however, limited the scope of their assessment to knowledge of HIV/sexually transmitted infections (STI) alone ( 11 – 16 ) or HIV/STI, contraception and limited reproductive physiology ( 17 ).
The present study will expand on previous Canadian work in two ways. First, it will assess student knowledge in multiple domains using an assessment questionnaire addressing all major topics included in Ontario’s high school human sexuality curriculum, including reproductive physiology throughout life (not just adolescence), HIV/STI, contraception and responsible sexuality including sexual consent. Second, unlike most previous Canadian studies, participants will be recruited from many different schools.
The objective of the present study was to conduct a preliminary assessment of sexual knowledge related to the learning objectives of Ontario’s minimally required high school sexual education course, among a sample of adolescents presenting to an emergency department who had completed their provincial high school sexual education requirements.
The present descriptive study used a convenience sample of adolescent patients (see patient eligibility below), from the paediatric emergency department of the London Health Sciences Centre, a tertiary care facility located in London, Ontario, whose catchment is two million people and which treats 37,500 patients annually. Ethics approval was obtained from the Health Sciences Research Ethics Board at the University of Western Ontario (London, Ontario) and the Clinical Research Impact Committee at the Lawson Health Research Institute (London, Ontario).
Questionnaire development
A questionnaire ( Appendix A ) designed to test expectations 1 through 4 outlined in the Ontario Ministry of Education’s Grade 9/10 Healthy Growth and Sexuality course ( Table 1 ) was developed (achievement of expectations 5 and 6 was not considered objectively testable by the authors.) Specific questions pertaining to each objective were developed using the Guidelines for Comprehensive Sexuality Education, 3rd Edition published by the Sexuality Information and Education Council of the United States (SIECUS) ( 18 ). This guideline, created by a national task force of health care professionals, educators and experts in adolescent development, contains recommendations for subject matter to be included in a comprehensive sexual education curriculum. Questions were also created using Canadian laws relevant to responsible sexuality ( 19 – 21 ) and Canadian health guidelines ( 22 – 25 ).
Questions were arranged into six categories: pregnancy; reproductive physiology and puberty; STI; contraception; HIV/AIDS; and sexuality and the law. Questions were true/false/unsure or multiple-choice. Participants were not asked about their personal experiences or values related to sexuality.
Additionally, participants used a seven-point Likert scale to rate the usefulness of various sources of sexual information ( Table 2 ), in which 1 = not at all helpful, 4 = somewhat helpful and 7 = extremely helpful.
Frequencies of respondents’ ratings of usefulness for six common sources of sexual information on a seven-point Likert scale
| Sexual education classes received in high school | 4 (2.0) | 7 (3.5) | 16 (8.0) | 58 (29.0) | 48 (24.0) | 48 (24.0) | 16 (8.0) |
| Sexual education classes received before high school | 22 (11.0) | 32 (16.0) | 48 (24.0) | 53 (26.5) | 25 (12.5) | 13 (6.5) | 3 (1.5) |
| Parents | 34 (17.0) | 35 (17.5) | 22 (11.0) | 39 (19.5) | 19 (9.5) | 19 (9.5) | 29 (14.5) |
| Friends | 20 (10.0) | 26 (13.0) | 31 (15.5) | 33 (16.5) | 37 (18.5) | 28 (14.0) | 22 (11.0) |
| Popular media (television, movies, magazines) | 41 (20.5) | 35 (17.5) | 29 (14.5) | 40 (20.0) | 29 (14.5) | 13 (6.5) | 10 (5.0) |
| Internet | 38 (19.0) | 29 (14.5) | 34 (17.0) | 35 (17.5) | 28 (14.0) | 14 (7.0) | 20 (10.0) |
Data presented as n (%)
Baseline characteristics were assessed, including age and sex; whether currently in school, and current/highest grade successfully completed; the number of high school health courses completed; whether the school in which these courses were taken was private or public, religious or secular; municipality in which the school was located; household structure (eg, two-parent, single-parent or alternative arrangement); and reason for presenting to the emergency department.
The questionnaire was piloted among a convenience sample of adolescents before distribution. Feedback was obtained about readability, time required to complete the survey, printed layout of the questionnaire, subject matter covered by the questions and whether any questions were perceived as invasive; further revisions were consequently made. The questionnaire took 10 min to 15 min to complete. Its Flesch Reading Ease score was 68% and its Flesch-Kincaid Grade level was 6.8.
Patient eligibility
Adolescent patients attending London Health Sciences Centre’s paediatric emergency department were considered eligible if they had completed at least one credit of health education in an Ontario high school (minimum provincial requirement), and triage scores upon presenting to the emergency department were neither resuscitative nor emergent (ie, Canadian Pediatric Triage and Acuity Scale score of 3 [urgent], 4 [less urgent] or 5 [non-urgent]). No age minimum was set as long as the educational requirement was met, but all participants were younger than 18 years of age (maximum patient age accepted by the paediatric emergency department). Exclusion criteria included incapacity to provide one’s own consent (assessed by the attending physician); insufficient fluency in written English (as self-reported by patient after inquiry); and acute pain, psychiatric or psychosocial crisis of such severity that recruitment was deemed inappropriate (assessed by the attending physician).
Questionnaire distribution
Once deemed eligible, the patient received the questionnaire with an accompanying letter of information. Completion of the questionnaire implied informed consent. Participants could complete the questionnaire in the presence of parents/guardians but were asked to refrain from discussion while completing it. However, respondents and parents/guardians were informed that upon return of the questionnaire, they would receive an answer key with explanations for each question that they could review together and take home. This allowed parents/guardians to let their child complete the questionnaire privately, knowing that the answer key would be available shortly for review and discussion.
If an eligible patient did not wish to participate, their reason for declining was documented.
Statistical analysis
Because this was a descriptive study without primary or secondary end points, a sample size calculation was not performed. It was decided that a sample size of 200 would obtain a sufficient cross-section of adolescents from different socioeconomic backgrounds and types of schools, while acknowledging that the convenience sample of emergency department patients may not be representative of the general adolescent population. Mean (± SD) scores were calculated for each question category and each question. Categorical variables were reported as percentages. A χ 2 test was used to assess associations between categorical variables; P<0.05 was considered to be statistically significant.
Of the 206 patients approached who met eligibility criteria, 200 agreed to participate. The six patients who declined cited disinterest in the subject matter as their reason. Respondents experienced a variety of presenting complaints, but the most common were musculoskeletal complaints (31%), minor trauma (13.5%) and abdominal pain (13.5%). Other baseline characteristics are summarized in Table 3 . Ages ranged from 14 to almost 18 years; the mean (± SD) age was 16±0.9 years. The mean current grade was 10.6±1.8. Fifty-six per cent were girls. Almost all were currently in school, with most attending a publicly funded school. Of the five available health/physical education courses offered in Ontario schools, almost one-half of respondents had completed one course (the minimum requirement) and approximately one-fifth had completed two courses.
Baseline characteristics of participants (n=200)
| Age, years, mean ± SD | 16.0±0.9 |
| Male participants | 88 (44) |
| Currently enrolled in school | 193 (96.5) |
| Current grade or highest grade completed, mean ± SD | 10.6±1.8 |
| Completed health and physical education courses (maximum available courses = 5) | |
| 1 | 94 (47) |
| 2 | 44 (22) |
| 3 | 26 (13) |
| 4 | 7 (3.5) |
| 5 | 2 (1) |
| Type of school attended | |
| Public | 170 (85) |
| Private | 7 (3.5) |
| Religiously based | 58 (29) |
| Secular | 129 (64.5) |
| Urban | 149 (74.5) |
| Rural | 39 (19.5) |
| Living situation | |
| With both parents | 129 (64.5) |
| With one parent | 43 (21.5) |
| Divides time between both parents | 9 (4.5) |
| Other | 19 (9.5) |
Data presented as n (%) unless otherwise indicated
Mean scores within each question category are summarized in Table 4 . Respondents correctly answered most questions relating to pregnancy physiology (79.6%), but performed less well on questions related to general reproductive physiology (61.6%). For example, 27% of respondents reported that pregnancy could result from oral sex, anal sex or mutual masturbation; 40% agreed with the statement that when a couple cannot conceive, the woman usually has a medical problem; and 55% could not identify when a woman is most likely to get pregnant during her menstrual cycle.
Mean scores within each question category
| Reproductive physiology and puberty | 6 | 3.7 (61.6) |
| Pregnancy | 9 | 7.2 (79.6) |
| Sexually transmitted infections | 7 | 5.5 (79.1) |
| HIV/AIDS | 2 | 1.0 (51.4) |
| Contraception | 3 | 1.3 (43.1) |
| Sexuality and the law | 6 | 4.0 (66.3) |
Respondents demonstrated good understanding of STI prevention (79.6% of questions correct). Each of the following were correctly identified by 75% to 90% of respondents: the need for regular sexual health examinations in both sexes; the potential for untreated STI to cause infertility or fetal harm during pregnancy; that STI are transmittable through oral sex; that condoms do not protect against all STI; and that STI may be asymptomatic. However, the majority (almost 60%) did not know that human papillomavirus may cause genital cancer in males in addition to females. Respondents also performed relatively poorly on questions related to HIV/AIDS (51.4% correct). Only 54% knew that HIV is not transmitted through all types of skin-to-skin contact, and when presented with a list of activities that included tattooing, piercing, sexual intercourse, intravenous drug use and blood transfusion, only 43% correctly selected blood transfusion as an uncommon method of contracting HIV in Canada.
Respondents held several misconceptions regarding common contraceptive methods (43.1% of questions correct): 78.5% erroneously agreed that the ‘morning-after pill’ terminates an existing pregnancy; 38% overestimated the contraceptive efficacy of male condoms with typical use; and 37.5% did not agree with the statement that oral contraceptives can be dangerous for women who smoke.
When presented with four scenarios, each depicting an instance of sexual assault, only 29.6% of respondents identified all four incidents as assault and 29.1% only recognized two or fewer as assault. Only 42.5% correctly identified Canada’s age of sexual consent as 16 years.
Girls scored better than boys in the pregnancy category (81.7% versus 76.9% correct; P=0.03) and the reproductive physiology/puberty category (64.5% versus 57.9% correct; P=0.04); other baseline characteristics did not correlate with any significant differences in scores. With respect to different types of schools attended (eg, private versus public, urban versus rural, religious versus secular) or the number of sexual education courses taken, no statistically significant differences were detected between the subgroups.
Respondents’ ratings of the usefulness of six common sources of sexual information are shown in Table 2 .
The present study built on previous Canadian assessments of student sexual knowledge in several important ways. Only one previous study attempted to assess sexual knowledge in multiple domains ( 17 ), and still failed to assess knowledge of reproductive physiology throughout life (including pregnancy), any STI other than chlamydia or HIV, abortion, sexual assault or sexual consent. Another weakness of earlier Canadian studies was that most recruited students from only one or two schools, making them vulnerable to selection bias. Three studies were performed on a national level with large samples ( 11 , 12 , 16 ) but all limited their assessment to knowledge of HIV/STI. The current study’s questionnaire was more comprehensive and included most of the topics recommended by an internationally recognized body of experts (ie, SIECUS).
Similar questionnaire-based studies have been performed in other nations to assess general sexual knowledge among youth ( 26 – 30 ), but the current study was the first to use a questionnaire systematically designed to correspond to our provincially mandated sexual education curriculum.
Sexual knowledge
Although respondents performed well on questions related to pregnancy physiology, they carried several concerning misconceptions related to general reproductive physiology, which could lead to negative outcomes throughout their lifespan.
Respondents were knowledgeable about STI prevention but performed less well on questions related to HIV/AIDS transmission. A previous study showed that most surveyed Canadian teenagers could identify major risk factors for HIV transmission (eg, sharing needles, unprotected sex, multiple sexual partners) ( 31 ). However, our results suggest that teenagers may have a poorer understanding of minor risk factors for HIV transmission (eg, that HIV is not transmitted through all skin-to-skin contact, and is rarely contracted via blood transfusions in Canada).
Many respondents held misconceptions about contraception that could lead to unsafe choices. Belief that the ‘morning-after’ pill causes abortion may lead to underuse of emergency contraception. Overestimation of the contraceptive efficacy of male condoms may explain why many sexually active Canadian girls use condoms without back-up contraception ( 32 ). Failure to understand the risk of smoking while taking oral contraceptives may increase the risk of thromboembolism in later adulthood.
No previous Canadian studies have assessed understanding of sexual consent laws among high school students. Canadians 15 to 24 years of age have an incidence of sexual victimization almost three times higher than the general population ( 33 ). Although learning to engage in ‘responsible sexual relationships’ is an expectation of Ontario’s sexual health curriculum ( 10 ), our findings suggest that Ontario students may have a poor understanding of sexual consent laws despite completing their course requirements. The relationship between this knowledge gap and the risk of sexual victimization could represent a potential area for future study.
Sources of sexual knowledge
High school sexual education classes received the highest average rating of usefulness among all listed sources. Ontario students appear to place great importance on their high school sexual health courses, which should motivate educators and policymakers to ensure that educational quality is maintained.
Interestingly, 17% of respondents rated the usefulness of the Internet as 6 of 7 or 7 of 7, putting it ahead of sexual health classes received before high school and popular media. A decade ago, many young Canadians were already using the Internet as their main source of sexual information ( 31 ). Given the recent explosion of social networking, further studies could explore how the ‘Facebook generation’ uses the Internet for sexual information, to determine whether it would be advantageous to incorporate modern online venues (eg, social networking sites) into sexual education.
Study limitations
The present study used a convenience sample of 200 adolescents from a southwestern Ontario paediatric emergency department. The emergency department setting permitted recruitment of students attending many different schools, an important advantage given the potential for variability in sexual education among schools. However, it is uncertain whether the sample was sufficiently representative to generalize the data to other adolescents in our region. Even more caution is needed before generalizing the data to adolescents from other parts of Canada where cultural, socioeconomic and municipal factors may affect local delivery of sexual education.
Teenagers did not have a separate space in which to complete the questionnaire without the presence of parents. Although parents were asked to refrain from discussing any questions with their children until provided with the answer key, their physical presence may have caused respondents to answer some questions differently. We observed that the study design frequently fostered healthy discussions about sexuality between participants and their parents; however, we must acknowledge that it may have also created bias.
Our questionnaire had an uneven distribution of questions from each category, which may have affected validity through its heterogeneity. For example, there were only two HIV-specific questions; therefore, answering one correctly produced a subscore of 50%; subscores may have been different had there been more HIV-specific questions.
Emergency department patients may also have other risk factors, such as lower socioeconomic status and/or more risk-taking behaviour ( 34 ), which may have affected their scores. While the results may not generalize well to youth outside of the emergency department, they at least suggest that this subset of students has gaps in sexual knowledge.
An important limitation was the use of a previously unvalidated assessment questionnaire, necessitated by the absence of standardized examinations or evaluation methods for sexual education courses in Ontario. Unlike the United States, where the SIECUS guidelines have long existed, Canada lacks national guidelines for content and delivery of school sexual education, which could have provided a benchmark for investigators to use when assessing the sexual knowledge of Canadian students. The Canadian Guidelines for Sexual Health Education, while providing general principles for administering sexual education, provide no specific suggestions for curriculum content or teaching strategies ( 35 ). In the absence of national standards and existing assessment tools, we had to create an original tool. A strength of the present study, however, was the systematic development of its questionnaire based on objective resources (ie, Ontario’s sexual education curriculum, SIECUS guidelines, and Canadian health laws and guidelines). Piloting the questionnaire among a sample of adolescents before its distribution was also a strength of the study; an additional pilot among health care providers experienced in working with adolescents may have further ensured accuracy and inclusion of an appropriate range of topics.
Although respondents disclosed the number of sexual education classes they had taken and the types of schools they attended (urban versus rural, private versus public, religious versus secular), the sample size was inadequately powered to detect significant differences between subgroups. Larger population-based studies are required to determine whether meaningful differences exist.
Finally, the present study could not assess the respondents’ knowledge of topics missing from Ontario’s sexual education curriculum, including sexual orientation, masturbation, sexual fantasy and sexual dysfunction. These topics are excluded despite SIECUS’s recommendations that they be included in any comprehensive sexual education program ( 18 ). Additional studies should assess understanding of these topics among Canadian adolescents, and intervention is required to incorporate these topics into Ontario’s curriculum.
The present study demonstrated significant gaps in sexual knowledge among a sample of Ontario adolescents who had completed their high school sexual education requirements. Subsequent studies are necessary to determine whether these findings can be replicated, and whether clinically meaningful differences exist between subgroups, by using a representative, population-based sample. Educators and policy-makers should consider conducting formal evaluations of high school sexual education courses that are currently being offered.
APPENDIX A. Children’s Hospital Sexual Education Assessment Survey

DISCLOSURE: The authors do not have any real, potential or perceived conflicts of interest to disclose. No honorarium, grant, or other form of payment was given to anyone to produce this article. Dr Maya M Kumar presented the results of this study in an oral platform presentation at the Canadian Paediatric Society Annual Conference on June 16, 2011, in Quebec City, Quebec.
Additional Resources
- Teacher Webinars and Workshops
- Ground Rules/Group Agreements
- Curriculum Overview
- Using the Lesson Plans
- Inclusive Language
- Instructional Methods
- Notifying Parents and Guardians
- Health Resources & Guest Speakers
- Comprehensive School Health
- Your Values
- Gender Identity & Expression
- Sexual Orientation
- Technology & Media
- Responding to Student Questions
- Student FAQs
- Submit a Student Question
- Managing Sensitive Issues
- Lesson Plan & Resource Finder
Differing Abilities
- CALM (10-12)
- Print Resources
- Alberta’s Education Act
- Best Practice Guidelines
Important Phone Numbers
No cost services available in many languages, emergency services.
Ambulance, Fire and Police.
Health Link
Free nurse advice and general health information.
A free, confidential, multilingual, information and referral system providing information on government and community-based health and social services. To see what is available in your region or community, visit.
Bullying Helpline
Advice or support on bullying.
Child Abuse Hotline
Call if you think a child is being abused or neglected by a parent or guardian.
Mental Health Helpline
Offers help for mental health concerns for Albertans.
Family Violence Info Line
Call if you (or someone you know) are going through family violence or abuse; if you have questions or want to find out about programs, resources and services.
Addiction Services Helpline
Help for problems with gambling, alcohol, tobacco and other drugs.
Related Resources
General health information.
- Also available in French: Des écoles en santé pour tous
- Healthy Parents, Healthy Children A practical guide to pregnancy and parenting, based on today’s knowledge, evidence and best practices. It’s available as a print and online resource for expectant parents, parents of children under 6 years of age and health care providers.
- Ready or Not Alberta A preconception health website for people aged 18-44 either planning, or not planning to become pregnant.
- Screening for Life Population-based breast, cervical, and colorectal cancer screening programs
- MyHealth Alberta A joint initiative by the Alberta Government and Alberta Health Services to give Albertans one place to go for health information they can trust. Health care experts across the province make sure the information is correct and up-to-date
Abuse & Assault
- 310-1818 available 24/7
- Online Chat available with trained staff, 8 am to 8 pm daily
- 1-866-403-8000 (call or text)
- Cyberbullying
- Homophobic Bullying
- Transphobic Bullying
- Government of Canada Children Online Information about keeping children safe online, including mobile use, social networking, cyberbullying and online exploitation
- Promoting Relationships & Eliminating Violence Network A national network of leading researchers and organizations, working together to stop bullying in Canada
- Alberta Teachers Association: Bullying information, prevention, teaching resources, videos and more Bullying Information and Research – Bullying Prevention – Resources at Alberta Teachers’ Association (libguides.com)
- COVID-19 and Sexual Health
- Sex Information and Education Council of Canada Provides a variety of resources for students and educators to support comprehensive sexual health education during the COVID-19 pandemic.
- Sex Information and Education Council of Canada Information for service providers and youth about sexual health education for Autistic Youth and Physically Disabled Youth
- Public Health Agency of Canada Questions & Answers: Sexual Health Education for Youth with Physical Disabilities Provides answers to common questions about sexual health education for youth with physical disabilities
- Talking About Sexuality in Canadian Communities A sexual health resource for providers of services to high-risk youth and youth with disabilities.
Indigenous Health
- Access the toll-free Helpline (1-855-242-3310) or the Online Chat, 24 hours a day, 7 days a week, to connect with a counsellor on-line.
- Society of Obstetricians and Gynaecologists of Canada Aboriginalsexualhealth.ca provides culturally safe and healing sexual health information for Aboriginal communities.
- Alberta Health Services Indigenous Health offers information about province-wide and zone-specific services for Indigenous people in Alberta.
Sexual Orientation/Gender Identity & Expression
- LGBTQ2S+/ Sexual and Gender Diversity
- Tools and Resources for Welcoming, Caring, Respectful and Safe Schools: Gay-Straight Alliances
- Alberta GSA Network A collective of resources specific to Alberta K-12 students, teachers and school staff, funded by the Government of Alberta
- Sexual Orientation and Gender Identity resources and information
- Information and resources on Diversity, Equity and Human Rights
- PRISM Toolkit for Safe and Caring Discussions about Sexual and Gender Minorities, for Elementary Schools
- PRISM Toolkit for Safe and Caring Discussions about Sexual and Gender Minorities, for Secondary Schools
- Camp fYrefly A national leadership retreat for lesbian, gay, bisexual, transgender, two-spirited, intersexed, queer, questioning, and allied youth
- Edmonton Public Schools and Edmonton Public Library Sexual Orientation and Gender Identity: Recommended Fiction and Nonfiction Resources for K-12 Schools
- Egale Canada Still in Every Class in Every School : Final report on the second national climate survey on homophobia, biphobia, and transphobia in Canadian schools. This report discusses the results of a national survey of Canadian high school students to investigate what life at school is like for students with sexual or gender minority status
- Questions & Answers: Sexual Orientation in Schools Answers common questions about sexual orientation in schools
- Questions & Answers: Gender Identity in Schools Answers common questions about gender identity in schools
- SOGI123 provides teachers with resources to support them in learning and teaching about sexual orientation and gender identity in their classroom.
- Fyrefly Institute at the University of Alberta includes resources for educators, students and families.
- Trans Equality Society of Alberta (TESA) TESA’s mission is to be a witness to and a voice for matters concerning trans Albertans.
- University of Alberta LGBTQ2S+ Teacher Resources (includes LGBTQ2S+ undergraduate and graduate courses)
Sexual & Reproductive Health Information
- MyHealth Alberta Answers common questions about the HPV vaccine
- Sexual and Reproductive Health Program and service information on sexual and reproductive health services in each zone, including pregnancy options, health topics and resources by topic and related websites. Includes information on abortion services
- Aboriginalsexualhealth.ca Culturally safe and healing sexual health information for Aboriginal communities.
- Sexandu.ca Provides guidance and advice to help individuals develop and maintain a healthy sexuality.
Sexual Health Education
- Alberta Health Services Sexual and Reproductive Health Education and consultation programs and services provided in each zone.
- Action Canada for Sexual Health and Rights Provides resources and information on advocacy, education, services and international and national policy engagement
- MediaSmarts Provides educational resources to help raise a media savvy generation
- Questions & Answers: Sexual Orientation in Schools Answers common questions about sexual orientation in schools
- Canadian Guidelines for Sexual Health Education Provides information to educators about key concepts in comprehensive sexual health education.
- Questions & Answers: Sexual Education in Schools Answers many questions about sexual health education in schools.
- Talking About Sexuality in Canadian Communities For service providers working with high-risk youth and youth with disabilities
- Technology & Media
- NeedHelpNow For youth who have been impacted personally by a sexual picture or video being shared by a peer or peers (sexting), cyberbullying personally or are supporting a friend.
- MediaSmarts Provides educational resources to help raise a media savvy generation.
Links to resources outside of the TeachingSexualHealth.ca website are provided for information only and do not imply an endorsement of views, products, or services. Although our staff regularly reviews these links, we can’t be certain that they are 100% credible since their content can be changed at any time.
What are students asking?
August 16, 2024
Winnipeg 22° C , Partly cloudy with wind
Full Forecast
- Advertising Contact
- Send a Letter to the Editor
- Staff biographies
- Submit a News Tip
- Subscribe to Newsletters
- Notifications
- Create Account
- Compact View
- About the E-Edition
- Winnipeg Free Press
- Community Review East
- Community Review West
- All Arts & Life
- Celebrities
- Environment
- Food & Drink
- Life & Style
- Science & Technology
- All Business
- Agriculture
- Personal Finance
- Manitoba’s Top Employers
- All Opinion
- Editorial Cartoon
- Letters to the Editor
- Auto Racing
- Blue Bombers
- High School
- Horse Racing
- Winnipeg Jets
- Manitoba Open
- Reader Bridge
- Free Press 101: How we practise journalism
- Advertising
- Carrier Positions & Retailer Requests
- FP Newspapers Inc.
- Internships
- Job Opportunities
- Local Journalism Initiative
- Retail Locations
- Staff Biographies
- Terms and Conditions
- Canada Sports Betting
- Online Casinos Canada
- Ontario Betting
- Responsible Gaming
- All Free Press Community Review News
- East Edition
- West Edition
- Classifieds
- All FP Features
- Business Hub
- Drink & Dine
- Health & Wellness
- Whiskers & Wings
- Sponsored Articles
- Credit Cards
- Credit Score
- Personal Loans
- Real Estate
- Side Hustles
- Property Listings
- Featured News
- Renovation and design
- Resale homes
- Newsletters
- Niigaan and the Lone Ranger
- Photo and Book store
- Become a Patron
- Privacy Policy
© 2024 Winnipeg Free Press
Quick Links
- Publications
- Sponsored Content
- Employee Code of Conduct Policy
- Supplier Code of Conduct Policy
- Report on Forced Labour and Child Labour in Supply Chains
Ways to support us
- Pay it Forward program
- Support Faith coverage
- Support Arts coverage
Replica E-Edition
Arts & Life
- Manitoba Moose
- Photo Galleries
Canstar Community news
- All Betting
Notification Settings
This browser doesn't support push notifications at the moment. Check browsers features, update your browser or try to use one from the list of recommended to manage your notifications settings:
- Firefox (27+)
- Google Chrome (30+)
- Safari ( MacOS 13+ with browser 16.1+ and iOS 16.4+ ) / Note make sure Push API support enabled under Settings > Safari > Advanced > Experimental Features
- Microsoft Edge
If you wish to manage your notification settings from this browser you will need to update your browser's settings for this site. Just click button below and allow notifications for this site
Note Safari 16.4+ working on iOS devices also need this site app to be installed at device's Home Screen for Push Notifications to work
Notifications are blocked for this site. If you wish to manage your notification settings from this browser you will need to update your browser's settings. Usually you'd need to click on site options icon to the left of address bar and change notifications preferences/permissions from there
Breaking News
Urgent and important stories
Recommended Reads
Noteworthy news and features
Advertisement
Learn more about Free Press Advertising solutions
Supreme Court keeps new rules about sex discrimination in education on hold in half the country
Advertise with us
WASHINGTON (AP) — The Supreme Court on Friday kept on hold in roughly half the country new regulations about sex discrimination in education, rejecting a Biden administration request.
Read this article for free:
Already have an account? Log in here »
To continue reading, please subscribe:
Monthly Digital Subscription
$19 $0 for the first 4 weeks *
- Enjoy unlimited reading on winnipegfreepress.com
- Read the E-Edition, our digital replica newspaper
- Access News Break, our award-winning app
- Play interactive puzzles
*No charge for 4 weeks then billed as $19 every four weeks (new subscribers and qualified returning subscribers only). Cancel anytime.
Read unlimited articles for free today:
The court voted 5-4, with conservative Justice Neil Gorsuch joining the three liberal justices in dissent.
At issue were protections for pregnant students and students who are parents, and the procedures schools must use in responding to sexual misconduct complaints.
The most noteworthy of the new regulations, involving protections for transgender students, were not part of the administration’s plea to the high court. They too remain blocked in 25 states and hundreds of individual colleges and schools across the country because of lower court orders.
The cases will continue in those courts.
The rules took effect elsewhere in U.S. schools and colleges on Aug. 1.
The rights of transgender people — and especially young people — have become a major political battleground in recent years as trans visibility has increased. Most Republican-controlled states have banned gender-affirming health care for transgender minors, and several have adopted policies limiting which school bathrooms trans people can use and barring trans girls from some sports competitions.
In April, President Joe Biden’s administration sought to settle some of the contention with a regulation to safeguard rights of LGBTQ+ students under Title IX, the 1972 law against sex discrimination in schools that receive federal money. The rule was two years in the making and drew 240,000 responses — a record for the Education Department.
The rule declares that it’s unlawful discrimination to treat transgender students differently from their classmates, including by restricting bathroom access. It does not explicitly address sports participation, a particularly contentious topic.
Title IX enforcement remains highly unsettled. In a series of rulings, federal courts have declared that the rule cannot be enforced in most of the Republican states that sued while the litigation continues.
In an unsigned opinion, the Supreme Court majority wrote that it was declining to question the lower court rulings that concluded that “the new definition of sex discrimination is intertwined with and affects many other provisions of the new rule.”
Justice Sonia Sotomayor wrote in dissent that the lower-court orders are too broad in that they “bar the Government from enforcing the entire rule — including provisions that bear no apparent relationship to respondents’ alleged injuries.”
Advertisement Advertise With Us
- Today's news
- Entertainment
- Deals and sales
- Royal fashion
- Celebrity fashion
- Shop the look
- Celebrity beauty
- Get the look
- My portfolio
- World indices
- Stocks: gainers
- Stocks: losers
- Stocks: most actives
- Top mutual funds
- Commodities
- Cryptocurrencies
- Saved screeners
- Equity screener
- Mutual fund screener
- ETF screener
- Business services
- Telecom and utilities
- Computer hardware and electronics
- Computer software and services
- Industrials
- Manufacturing and materials
- Consumer products and media
- Diversified business
- Retailing and hospitality
- Real estate
- Currency converter
- Fantasy football
- Fantasy hockey
- Fantasy basketball
- Fantasy baseball
- Scores/schedules
- Premier League
- Champions League
- Leaderboard
- Yahoo Sports Experts
- Privacy Dashboard
Supreme Court keeps new rules about sex discrimination in education on hold in half the country
WASHINGTON (AP) — The Supreme Court on Friday kept on hold in roughly half the country new regulations about sex discrimination in education, rejecting a Biden administration request.
The court voted 5-4, with conservative Justice Neil Gorsuch joining the three liberal justices in dissent.
At issue were protections for pregnant students and students who are parents, and the procedures schools must use in responding to sexual misconduct complaints.
The most noteworthy of the new regulations, involving protections for transgender students, were not part of the administration's plea to the high court. They too remain blocked in 25 states and hundreds of individual colleges and schools across the country because of lower court orders.
The cases will continue in those courts.
The rules took effect elsewhere in U.S. schools and colleges on Aug. 1.
The rights of transgender people — and especially young people — have become a major political battleground in recent years as trans visibility has increased. Most Republican-controlled states have banned gender-affirming health care for transgender minors, and several have adopted policies limiting which school bathrooms trans people can use and barring trans girls from some sports competitions.
In April, President Joe Biden’s administration sought to settle some of the contention with a regulation to safeguard rights of LGBTQ+ students under Title IX , the 1972 law against sex discrimination in schools that receive federal money. The rule was two years in the making and drew 240,000 responses — a record for the Education Department.
The rule declares that it’s unlawful discrimination to treat transgender students differently from their classmates, including by restricting bathroom access. It does not explicitly address sports participation , a particularly contentious topic.
Title IX enforcement remains highly unsettled. In a series of rulings , federal courts have declared that the rule cannot be enforced in most of the Republican states that sued while the litigation continues.
In an unsigned opinion, the Supreme Court majority wrote that it was declining to question the lower court rulings that concluded that “the new definition of sex discrimination is intertwined with and affects many other provisions of the new rule.”
Justice Sonia Sotomayor wrote in dissent that the lower-court orders are too broad in that they “bar the Government from enforcing the entire rule — including provisions that bear no apparent relationship to respondents’ alleged injuries.”
The Associated Press
Latest Stories
Forest fires burning 3 km from sask. power plant, but officials say disruption is unlikely.
Forest fires continue to rage in northeast Saskatchewan, causing evacuations in communities like Sandy Bay.The fires are also close to the Island Falls hydroelectric station, which supplies power to most of the province's northeast.SaskPower spokesperson Scott McGregor said the wildfire is three kilometres from the station and has remained at roughly that distance for the past few days. He said the station is surrounded by fire breaks, and staff are regularly watering down all relevant buildings
Army chaplain injured in stabbing at barracks
Fr Paul Murphy has been taken to hospital in Galway, where his injuries are said to be serious but not life-threatening.
- Why this Ad?
- I don't like this ad
- Go ad-free*
Queen Rania shares glimpse inside new mother Princess Rajwa's pristine home with baby Iman
Queen Rania of Jordan cuddled Crown Prince Hussein and Princess Rajwa's baby Iman in a low-key photo which could have been taken inside Raghadan Palace.
Scaramucci: Trump Is ‘Coming to Grips’ With Losing the Election
Anthony Scaramucci, Donald Trump’s one-time White House communications director, thinks his former boss is “coming to grips” with the possibility that he’ll lose the election and is consequently “growing darker.”“Will be a rough 81 days,” Scaramucci added in an X post Thursday, referring to the time left until Election Day in November. His comment came as Trump spoke at an hour-long press conference at his golf club in Bedminster, New Jersey, in which the Republican nominee explicitly rejected p
Joe Biden Shades Trump With 1 Brutally Blunt Piece Of Advice
The president went into Dark Brandon mode when asked about his predecessor.
OOPS! Trump Accidentally Hands Kamala Harris And Gavin Newsom A Major Compliment
The former president's latest attempt at an insult quickly backfired.
Biden Hits Trump With A New Nickname, Slams GOP For Refusing To Lower Drug Prices
The president also joked about his own age during his first joint appearance with Kamala Harris since dropping out of the race.
Biden Unloads on Trump Like Never Before
Upper Marlboro, Maryland — President Joe Biden has come out swinging like never before against his one-time opponent, Donald Trump.“The guy we’re running against, what’s his name?” Biden asked as the crowd laughed during his first campaign trail appearance with Democratic nominee Kamala Harris on Thursday. “Donald Dump? Or Donald Whatever?”In a fiery 22-minute speech at a Prince George’s County gymnasium in Maryland, Biden roared about his policy accomplishments, poked fun at concerns about his
Trump is either delusional or confused. He's unfit for the White House either way
Donald Trump is either deranged or at least delusional. Maybe confused, but that's just as worrisome. What rational mind can't remember the details of plummeting from the sky and facing possible death in a helicopter?
Trumpworld scrambling to clean up ‘mess’ after ex-president’s angry texts to megadonor
Those close to the former president privately told reporters he has acted out of anger recently
Trump draws fire for remarks about Medal of Honor recipients
Former president Donald Trump sparked criticism when he said the Presidential Medal of Freedom, the nation's highest civilian award, is "much better" than the Medal of Honor, the nation's highest military honor, because soldiers are in "bad shape" or dead when they receive it – comments Trump's campaign suggested were misinterpreted. During an event at his Bedminster, NJ estate Thursday night, which was about antisemitism, Trump called attention to a major donor, Miriam Adelson – the widow of his friend and business mogul Sheldon Adelson – upon whom he bestowed the Medal of Freedom in 2018.
Trump's Bleak Stock Market Prediction Instantly Undermined By Fox News Graphic
The former president made some scary claims about the economy at the same time stock prices were soaring on Thursday.
Humiliation for Putin as Over 100 Troops Raise White Flag on Russian Soil
Ukrainian forces captured over 100 Russian troops in the largest single surrender since the start of the war two and a half years ago, according to multiple reports.The latest victory is part of a surprise incursion launched by Ukraine into Russian territory earlier this month. The surrender will not please Russian President Vladimir Putin, who was already visibly rattled during a testy televised meeting with officials earlier this week.The Ukrainian online newspaper Ukrainska Pravda posted a vi
Hidden-camera video shows Project 2025 co-author discussing his secret work preparing for a second Trump term
Russell Vought, a co-author of Project 2025, was caught on a secretly recorded video saying that Trump’s denials of any connection with the conservative policy blueprint were politics.
Harris says in fundraising email she ate ‘a family-sized bag of nacho Doritos’ on night of Trump election
Vice President Harris said in a fundraising email sent Friday that she ate “a family-sized bag of nacho Doritos” the night of the 2016 election. In the email, Harris questions whether recipients remember their own emotions and reactions to Donald Trump’s win over Democratic nominee Hillary Clinton in that presidential cycle. “It was election night…
CNN Fact-Checker Exposes 2 New 'Egregiously Wrong' Trump Claims
"There was a whole bunch of lying," Daniel Dale summarized after watching the former president's press conference.
Seth Meyers Stunned By Trump's 'Olympic-Level Idiot' Level Of Self-Sabotage
"I owe Trump an apology," the "Late Night" host said.
'Daily Show' Draws A Wicked Reminder For Trump And His Artistic Wishes
Desi Lydic questioned why the former president would "really" need a new sketch artist.
Corey Lewandowski Returns To Advise Trump, Immediately Screws Up
It involved the word "couch," naturally.
Ukraine strikes ferry crossing in occupied Crimea and vessel in Russia
Explosions were reportedly heard across Crimea in the early hours of the morning.
- Newsletters
- News Insiders
Supreme Court keeps new rules about sex discrimination in education on hold in half the country

By The Associated Press
Posted Aug 16, 2024 07:14:09 PM.
Last Updated Aug 16, 2024 07:15:21 PM.
WASHINGTON (AP) — The Supreme Court on Friday kept on hold in roughly half the country new regulations about sex discrimination in education, rejecting a Biden administration request.
The court voted 5-4, with conservative Justice Neil Gorsuch joining the three liberal justices in dissent.
At issue were protections for pregnant students and students who are parents, and the procedures schools must use in responding to sexual misconduct complaints.
The most noteworthy of the new regulations, involving protections for transgender students, were not part of the administration’s plea to the high court. They too remain blocked in 25 states and hundreds of individual colleges and schools across the country because of lower court orders.
The cases will continue in those courts.
The rules took effect elsewhere in U.S. schools and colleges on Aug. 1.
The rights of transgender people — and especially young people — have become a major political battleground in recent years as trans visibility has increased. Most Republican-controlled states have banned gender-affirming health care for transgender minors, and several have adopted policies limiting which school bathrooms trans people can use and barring trans girls from some sports competitions.
In April, President Joe Biden’s administration sought to settle some of the contention with a regulation to safeguard rights of LGBTQ+ students under Title IX , the 1972 law against sex discrimination in schools that receive federal money. The rule was two years in the making and drew 240,000 responses — a record for the Education Department.
The rule declares that it’s unlawful discrimination to treat transgender students differently from their classmates, including by restricting bathroom access. It does not explicitly address sports participation , a particularly contentious topic.
Title IX enforcement remains highly unsettled. In a series of rulings , federal courts have declared that the rule cannot be enforced in most of the Republican states that sued while the litigation continues.
In an unsigned opinion, the Supreme Court majority wrote that it was declining to question the lower court rulings that concluded that “the new definition of sex discrimination is intertwined with and affects many other provisions of the new rule.”
Justice Sonia Sotomayor wrote in dissent that the lower-court orders are too broad in that they “bar the Government from enforcing the entire rule — including provisions that bear no apparent relationship to respondents’ alleged injuries.”
The Associated Press
Top Stories

HALIFAX — The family of a Nova Scotia firefighter who died during a 2019 training session is stepping up its push for reform of a firefighting school after learning he had raised concerns about the equipment...

East Hants District RCMP has charged a teacher at a school for sexual offences involving a student. On June 3, Mounties received a report of inappropriate contact with a student by an employee working...
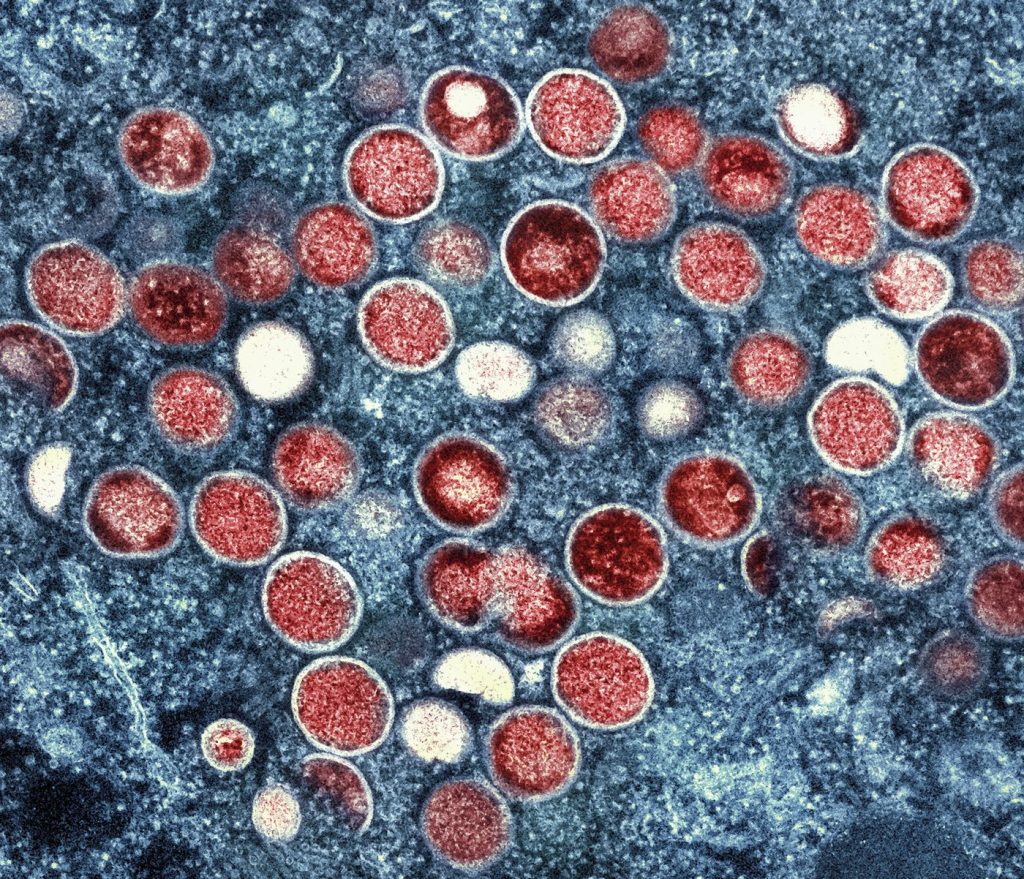
A public health official in Nova Scotia says there are no known active cases of mpox in the province. Earlier this week, the World Health Organization declared the mpox outbreaks in Africa a global...

Hurricane Ernesto is not expected to have much of an impact on the weather in Nova Scotia next week. "There's high confidence in the forecast models that the storm will track to the southeast of Sable...
Most Watched Today

Stock markets rebound from early August losses, Canopy Growth Corporation will get a new CEO next year and Air Canada pilots are wrapping up a strike vote next week. Kris McCusker explains.

For the first time in almost a month, Jasper residents will be able to go home Friday. As Sean Amato reports, officials are warning some may only be able to visit. #Jasper #abfire

New polling for CityNews finds while 4 in 10 say they might possibly consider voting Liberal after a shuffle, a majority say they wouldn't. One pollster says the desire for change is unlike anything he's seen in 35 years.

Protests are escalating across India after a young female doctor was raped and murdered. Michelle Mackey reports on the growing calls for justice and systemic change.

Gaza’s health ministry says more than 40,000 people have now been killed, as Israel reports its military has "eliminated" more than 17,000 Palestinian militants in Gaza since the start of the war.
Adjust preferences
With your consent we may collect cookies and information to enhance our service, and improve your experience.
These cookies and data are essential for browsing our website and allowing services. Examples include, session, authentication, and security cookies.
These cookies and data enable the website to provide enhanced functionality and personalized content.
These cookies and data inform us which pages are most informative and engaging via analytics.
These cookies may track data across websites for marketing and interest-based advertising to provide personalized content, offers, and advertisements.
- Friends of SHORE
- Get Involved

SEXUAL HEALTH EDUCATION
SHORE Centre offers evidence-based, up-to-date, comprehensive sexual health education. Our programs follow the Canadian Guidelines for Sexual Health Education produced by the Public Health Agency of Canada. These guidelines aim to improve sexual health outcomes including self-esteem, safety and pleasure, while reducing negative outcomes such as unintended pregnancies, sexually transmitted infections and harmful relationships.
These improved outcomes are reached by following three key elements: Information, Motivation & Behaviour, known together as the IMB Model. This model highlights the fact that simply providing people with information is not enough to encourage change, and that information must be followed by encouraging motivation and behavioural skills to be effective. Often this model is implemented with activity-based lessons.
We are committed to providing programs that:
• Focus on harm reduction and prevention of unplanned pregnancies, STIs, sexual assault and unhealthy relationships. • Provide accurate, up-to-date evidence based information. • Include activities that address social pressures that influence sexual behaviour. • Provide opportunities for participants to practice skills associated with communication, negotiation, and refusal skills. • Are interactive whenever possible to encourage personalization of the information provided. • Are age appropriate in the manner of delivery, content, stated outcomes and sexual experience of the participants. • Are sensitive to age, culture, ethnicity, racial identity, faith, ability, gender and orientation. • Supplement education happening in the school and home, and generate dialogue between parents/caregivers and their children.

Accurate and inclusive Sexual Health Workshops for all ages delivered in schools and with local community groups.

Peer Theatre Education , an interactive play for youth around sexual health and relationships.
Just4Me , an 8 week youth program delivered in schools and community centres.

Sex-Ability , a program for youth and adults with developmental disabilities.
Newcomer Health Programs provided in several languages around family planning and healthy relationships.
Learn more about our sexual health education workshops and programs
Why is sex and sexuality education taught in Australian schools?

From pre-school to year 12, sexual education is part of the school curriculum in Australia. Source: Getty / Lincoln Beddoe
Get the SBS Audio app
Other ways to listen, sex ed in schools is controversial, but experts say it's vital for young people to learn about their bodies, identities, and healthy relationships. why are some parents concerned, latest podcast episodes.

What is genocide?

Islamophobia in everyday life

Is immigration worsening the housing crisis?
Online child sexual exploitation is now at epidemic levels and that has police concerned
International and domestic organized crime groups capitalizing on vulnerable youths, say police.

Social Sharing
Police finally had a name — and the suspect was one of their own.
For months, Alberta's Internet Child Exploitation (ICE) unit sleuthed someone who uploaded two videos showing child sexual exploitation to Snapchat. In late April, investigators learned the suspect's identity: Evan Peacock, a 33-year-old RCMP constable stationed in St. Paul, Alta.
Investigators searched his home, seizing evidence for the forensics team. Peacock, who served more than three years, was arrested and charged with several child pornography offences.
He was released from custody with conditions and suspended with pay. But Alberta RCMP charged him again in June, following an investigation into a man soliciting sex with girls online.
- Child pornography charges laid against Alberta RCMP officer
The incidents, which have yet to be proven in court, fall into the realm of online child sexual exploitation — an umbrella term for numerous forms of abuse, such as child pornography, sextortion and online grooming.
It is a growing space that is becoming more difficult to police, experts say. Tens of thousands of cases are reported to Canadian law enforcement, including Albertan agencies, but countless go unreported.
- Have a story or knowledge to share about online child sexual exploitation? Please fill out this form so CBC News can connect with you. Tips can also be sent to the reporter (email below).
"It really exploded when we had the [COVID-19] pandemic," said Signy Arnason, acting executive director of the Canadian Centre for Child Protection.
"We had more kids online, increased amount of time — and equally more offenders online looking to harm kids in some capacity."
ICE case intake skyrockets
ICE, a faction of Alberta Law Enforcement Response Teams (ALERT), investigates offences involving child pornography, computer-related child sexual abuse, luring over the Internet, voyeurism and child sex trafficking.
Its cases have more than tripled in six fiscal years, from about 1,050 in 2018 to more than 3,800 in 2023, according to its latest annual report.
Data provided by ALERT shows its ICE unit laid about 1,280 charges throughout the last three fiscal years. More than two-thirds were related to child porn — or, child sexual abuse material. Each incident can result in multiple charges.
Reports of online child sexual exploitation and abuse can come from various sources, such as police complaints and Cybertip — the national tipline operated by the Canadian Centre for Child Protection.
Social media companies and international agencies, such as the National Center for Missing and Exploited Children in the United States, may also flag incidents or materials they detect.
The RCMP's National Child Exploitation Crime Centre received nearly 103,000 total complaints and reports in fiscal 2022 — an increase of 26 per cent from the previous year, an RCMP spokesperson said.
- Child sex exploitation is on the rise in Canada during the pandemic
- Online child exploitation complaints in Alberta on the rise, police say
Cybertip data shows reports from Alberta grew each year from 2020 to 2023 — the only years for which its publicly available data accounts.
A fraction of those reports were forwarded to local law enforcement or child welfare agencies, but that proportion has also grown. Of the nearly 1,500 reports from Alberta last year, one-third were passed along to such organizations, data shows.
Alberta's judicial system, meanwhile, is hearing hundreds of more cases related to online child sexual exploitation, according to data obtained from the justice ministry.
CBC News requested data relating to cases heard in the Court of Justice and Court of King's Bench, from fiscal 2013 to 2023, that involved charges often associated with online child sexual exploitation, such as luring and child pornography offences.
The courts heard roughly 1,500 such cases combined in fiscal 2013, data shows. The caseload reached more than 2,500 in fiscal 2021 — the most during the decade requested.
Last year, the courts heard almost 2,200 cases.
Sexual extortion on the rise
Sexual extortion, or sextortion, is the most rampant exploitation crime right now, officials say. Sgt. Kerry Shima, acting head of the ICE unit, described sextortion as an epidemic.
"It's completely out of control — and, disturbingly, it's probably the most underreported crime that I've ever seen," Shima said. A conversation sparked on social media can turn sexual, leading to requests for nude photos or sexual videos. But now, more offenders are going further: once they receive the abusive material, the threats begin.
Organized crime groups are perpetrating sexual extortion schemes more often, forcing police to manoeuvre international law to go after them.
- Sextortion: Ad campaign targets youth as reports of online sexual exploitation increase
More than 6,500 sextortion cases have been reported to the Canadian Centre for Child Protection in the past 18 months, Arnason told CBC News in June.
From 2021 to 2023, the Canadian Anti-Fraud Centre — a federal agency that tracks fraud and identity theft — received 1,715 reports of extortion that started on social media.
The anti-fraud centre believes most of those cases, which affected people of all ages, were sextortion incidents — but those are just the ones it knows about.
It estimates only five to 10 per cent of fraudulent incidents are reported.
Historically, financial sextortion was targeted toward adults, but now teenagers — particularly boys — are the main victims, Arnason said.
As such schemes garner success, more people are trying to pull them off because money can be made, she said.

"Part of the challenge is that a lot of these schemes are incredibly successful," Arnason said.
Working within borders
Under international law, the involvement of criminal organizations based outside of the country can obstruct Canadian police during investigations, said Robert Currie, a law professor at Dalhousie University in Halifax.
Countries can be "very picky" when it comes to international law enforcement, he said. Each country has its version of criminal law, so they're careful when interacting with other countries in that realm.
"International law says we do the criminal investigation on our soil and you do it on your soil," Currie said. "If there are solutions, they're around co-operation."
Canada, for example, has the Mutual Legal Assistance in Criminal Matters Act .

The legislation allows for Canada to obtain court orders on behalf of other countries for things like search and seizure, gathering evidence and extradition.
Canada can still help countries with which it does not have a treaty, but certain conditions have to be met and the scope is more limited, according to the justice ministry's website .
Currie noted, however, that law enforcement often communicate informally across borders.
"They feed each other information. To an extent, they feed each other evidence — and it's got to be this kind of cross-border co-operation model, because of the limits on enforcement," he said. "These are hard cases because of that."
Alberta's ICE unit navigates similar channels, but co-operation varies depending on the location, Shima said.
American law enforcement, as well as intelligence alliances such as the Five Eyes — between Australia, Canada, New Zealand, the United Kingdom and the United States — co-operate well, he said.
Investigations alongside countries with no agreements are more difficult, he said.
"The Internet has no boundaries," Shima said.
"It's not to say that [arrests] can't happen. It's just very complicated sometimes."
In cybercrime cases, international law acknowledges that a crime can be committed in two jurisdictions — the offender being in one, the victim in another, Currie said. Canadian police cannot enter another country, but the offender — when arrested — can be tried in Canada.
- Aydin Coban sentenced to 13 years for sexual extortion of Amanda Todd
- Dutch man who sexually extorted B.C. teen Amanda Todd given 6-year sentence in Netherlands
Currie highlighted the case of Amanda Todd, a teenager from B.C., who killed herself in 2012 after being cyberbullied and sexually extorted by Aydin Coban, a Dutch man in the Netherlands.
The B.C. Supreme Court sentenced Coban to 13 years in prison in 2022. Conversion hearings were held in the Netherlands in 2023 to align the punishment with Dutch law. A Dutch judge sentenced him to six years.
Hurdles to overcome
Alberta's ICE unit has seven to nine investigators working at any given time, spread throughout the province.
Once it receives a report, Shima said, the agency will triage it based on location, then further by seriousness.
"We have to because we have too many files for us to work on all at once," he said.
The unit deals with a lot of child pornography collectors and traders, sometimes seizing large collections of abusive material, Shima said. But victims of sextortion are a higher priority.
With few investigators, the ICE unit manages investigations to avoid overwhelming the forensic examination teams and create court delays, Shima said.
Currie echoed that Canadian police don't necessarily have the resources needed for cybercrime investigations.
Officers need better training on international law, such as who to contact in a specific country, and law enforcement agencies need greater cyber expertise, he said.
- Ottawa to create regulator to hold online platforms accountable for harmful content: sources
"There will never be less of these cases," Currie said.
"This is a growth industry — and organized crime gangs are as large and sophisticated as they have ever been."
If you, or someone you know, have been affected by online child sexual exploitation, there are some resources to which you can report the incident or get support:
- Local police
- Crime Stoppers: online or 1-800-222-8477
- Cybertip: online or 1-866-658-9022
- Kids Help Phone : 1-800-668-6868
- The Suicide Crisis Helpline : call or text 9-8-8
If in immediate danger, call 9-1-1.
ABOUT THE AUTHOR

Nicholas Frew is a CBC Edmonton reporter, who specializes in producing data-driven stories. Hailing from Newfoundland and Labrador, Frew moved to Halifax to attend journalism school. He has previously worked for CBC newsrooms in Manitoba and Saskatchewan. Before joining CBC, he interned at the Winnipeg Free Press. You can reach him at [email protected].
Related Stories
- 10 years after Tina Fontaine's murder, lead investigator maintains police charged right person
- Police investigating attacks on 2 men who used dating app Grindr in Sherbrooke, Que.
- Officer wellness, community relationships priorities for new LaSalle police chief
- N.S. man sentenced to 4 years in prison for historical sexual assault
- Suspicious fire causes millions in damages at Vancouver Walmart: police
Advertisement
Supported by
JD Vance, an Unlikely Friendship and Why It Ended
His political views differed from a transgender classmate’s, but they forged a bond that lasted a decade — until Mr. Vance seemed to pivot, politically and personally.
- Share full article

By Stephanie Saul
Stephanie Saul, who covers education, reviewed about 90 emails and text messages spanning between 2014 and 2017.
When his book, “Hillbilly Elegy,” was published in 2016, JD Vance sent an email apologizing to a close friend from his Yale Law School days. The friend identified as transgender, but Mr. Vance referred to them in the book as a lesbian.
Listen to this article with reporter commentary
“Hey Sofes, here’s an excerpt from my book,” Mr. Vance wrote to his friend, Sofia Nelson. “I send this to you not just to brag, but because I’m sure if you read it you’ll notice reference to ‘an extremely progressive lesbian.’”
“I recognize now that this may not accurately reflect how you think of yourself, and for that I am really sorry,” he wrote. “I hope you’re not offended, but if you are, I’m sorry! Love you, JD.”
Nelson wrote back the same day, calling Mr. Vance “buddy” and thanking him for “being sweet,” adding, “If you had written gender queer radical pragmatist, nobody would know what you mean.” Nelson asked for an autographed copy, then signed off with, “Love, Sofia.”
That exchange is from a series of emails between two friends, part of a close-knit group of 16 students who remained together throughout their first law school semester in the fall of 2010. As now-Senator Vance seeks the vice presidency, Nelson has shared about 90 of their emails and text messages, primarily from 2014 through 2017, with The New York Times.
We are having trouble retrieving the article content.
Please enable JavaScript in your browser settings.
Thank you for your patience while we verify access. If you are in Reader mode please exit and log into your Times account, or subscribe for all of The Times.
Thank you for your patience while we verify access.
Already a subscriber? Log in .
Want all of The Times? Subscribe .

IMAGES
COMMENTS
Activists rally against so-called gender ideation being taught in schools, marched from Barbara Hall Parkette to Queens Park in Toronto on Wednesday. Sexual education programs designed to foster ...
Parents can now opt their child out of sex-ed lessons with a new policy put into place - this must be completed by Nov. 30. The new curriculum has a stronger and earlier emphasis on mental ...
Advocate at the local, provincial and territorial levels for the use of the Canadian Guidelines for Sexual Health Education as a framework for developing a broadly-based sexual health curriculum, which includes sexual orientation and gender identity.; Establish clear school policies to support teachers in the discussion and delivery of broadly-based sexual health education in the classroom.
Sex education, mandated in most Canadian schools, aims to teach youth about healthy sexual expression and relationships. However, programme delivery may vary widely, and sex education tends to focus on pregnancy and disease prevention and less on interpersonal issues such as relationships and violence. Sex education research tends to follow suit, focusing on dichotomous health outcomes rather ...
The 2019 Canadian guidelines for sexual health education by Sex Information and Education Council of Canada (SIECCAN) are meant to be a guide for educators and policy makers when it comes to comprehensive sexuality education in Canada. The 2019 edition includes new content on the importance of comprehensive sex-ed in Canada, a list of key ...
A National Parent Survey conducted by the Sex Information and Education Council of Canada in 2020 found that 90 per cent of parents surveyed in B.C. agreed that sexual health education should be ...
A large study by Alex McKay, executive director of the Sex Information and Education Council of Canada, and colleagues found that 87 per cent of Ontario parents agreed that sexual health education ...
The goal was and is to prepare knowledgeable, inclusive educators and improve the experience of those who may be marginalized because of their sexual orientation and/or gender identity in our programs, classrooms and workplaces. None of this work has taken place in a vacuum. Our work augments earlier work within the Faculty of Education and ...
Alex McKay of the Sex Information and Education Council of Canada said the new program is a "significant move" toward bringing Ontario in line with some of the other provinces in providing ...
These Questions and Answers are designed to support the implementation of the Canadian Guidelines for Sexual Health Education 2. The Guidelines are based on evidence that broadly-based sexual health education should reflect the diverse needs and realities of all people in ways that are age-appropriate, evidence-based, scientifically accurate ...
sources of support with respect to sexual health (for example, parents, health professionals, in-school resources, local community groups and religious, spiritual, and cultural leaders) gender identity, gender expression and sexual orientation, and to identify factors that can help all young people to develop positive personal identities
In Canada, education and healthcare are provincial jurisdiction, and so each province has differing education systems and different sex education curricula. In Ontario, some form of sex education has been present in schools since the early 1900s. From 1925 to 1933, the Ontario Health Department charged nurse Agnes Haygarth to give lectures on ...
Sex Information and Education Council of Canada, SIECCAN. The Canadian Guidelines for Sexual Health Education provide guidance to educators and policy makers for the development and evaluation of comprehensive evidence-based sexual health education in Canada. The revised 2019 Guidelines include new content: a section documenting the importance ...
The Ontario government's revised sex-education curriculum for elementary schools includes instruction on health, cyber safety and consent, and requires school boards to allow parents to exempt ...
Most 15- to 17-year-olds in Canada reported having at least one source of sexual health information (96.6%). More than half identified school (55.6%) and parents or guardians (51.2%) as sources of sexual health information. The internet (45.9%), friends (36.2%), and health care professionals (20.9%) were other common sources.
Approaches to sexuality education in Ontario, Canada are heavily contested as conversations continue regarding the place of comprehensive sexuality education within Ontario school boards and how such debates construct children and childhood (e.g. Bialystok, 2018, 2019; Bialystok et al., 2020; Davies, 2021; Davies and Kenneally, 2020; Grace, 2018). ...
The Sex Information & Education Council of Canada (SIECCAN) is a not-for-profit charitable organization established in 1964 that works with health professionals, educators, community organizations, governments, and corporate partners to promote sexual and reproductive health.
The grade at which children are told about STIs and their prevention: Ontario: Grade 7. B.C.: Grade 6. Alberta: Grade 6. Saskatchewan: Grade 6. Manitoba: Grade 7. Quebec: Between 12-17 years old ...
In Canada, education is under provincial jurisdiction and almost every province's high school curriculum contains formal sexual education. Within the province of Ontario, sexual education is a subcomponent of health and physical education courses; each course is comprised of approximately 110 h of instruction.
Counterprotesters to the One Million March for Children Canada, by activists against so-called gender ideation being taught in schools, marched from Barbara Hall Parkette to Queens Park in Toronto on Wednesday. ... "What sex education does in our schools is actually give our children education and information. And that's not indoctrination ...
310-1818 available 24/7. Online Chat available with trained staff, 8 am to 8 pm daily. Alberta's One Line for Sexual Violence is available to anyone in Alberta who is looking for support or referrals to specialized sexual assault services. 1-866-403-8000 (call or text)
Breaking News, Sports, Manitoba, Canada. WASHINGTON (AP) — The Supreme Court on Friday kept on hold in roughly half the country new regulations about sex discrimination in education, rejecting a ...
Ontario, Canada's most populous province, introduced a new sex-ed curriculum in 2015 in an attempt to modernise the programme in light of many changes to Canadian society and the growth of social ...
WASHINGTON (AP) — The Supreme Court on Friday kept on hold in roughly half the country new regulations about sex discrimination in education, rejecting a Biden administration request.. The court voted 5-4, with conservative Justice Neil Gorsuch joining the three liberal justices in dissent. At issue were protections for pregnant students and students who are parents, and the procedures ...
In April, President Joe Biden's administration sought to settle some of the contention with a regulation to safeguard rights of LGBTQ+ students under Title IX, the 1972 law against sex discrimination in schools that receive federal money. The rule was two years in the making and drew 240,000 responses — a record for the Education Department.
SHORE Centre offers evidence-based, up-to-date, comprehensive sexual health education. Our programs follow the Canadian Guidelines for Sexual Health Education produced by the Public Health Agency of Canada. These guidelines aim to improve sexual health outcomes including self-esteem, safety and pleasure, while reducing negative outcomes such as unintended pregnancies, sexually transmitted ...
From pre-school to year 12, sexual education is part of the school curriculum in Australia. Source: Getty / Lincoln Beddoe
Online child sexual exploitation is a growing problem worldwide — and Alberta is no exception. With limited resources, police are forced to triage the most serious cases and, more often, work ...
The cases will continue in those courts. The rules took effect elsewhere in U.S. schools and colleges on Aug. 1. The rights of transgender people — and especially young people — have become a ...
Stephanie Saul, who covers education, reviewed about 90 emails and text messages spanning between 2014 and 2017. Published July 27, 2024 Updated July 29, 2024